Jennifer Harman, St. Jude Children's Research Hospital, Memphis, Tennessee
Melissa Buchholz, University of Colorado School of Medicine; Children's Hospital Colorado, Aurora, Colorado
Obianuju O. Berry, Columbia University Medical Center, New York, New York

Abstract
Many hospitals and academic medical settings lag behind in promoting key initiatives focused on advancing maternal, infant, and early childhood mental health. Yet, systems are dynamic and change is possible. This article highlights Fellows’ efforts to infuse maternal, infant, and early childhood mental health understanding and approaches into medical settings. Ample opportunities exist to engage with families of young children in medical settings, in a culturally sensitive way, to meet their mental health and developmental needs.
Mental health providers are traditionally tasked with treating specific diagnoses, responding to concerns, and reacting to crises. There is less of a focus on intervening before problems exist and equipping families with tools and strategies to prepare them to support their child in reaching their optimal developmental potential. However, research has demonstrated the benefit of early identification and intervention for young children and the positive long-term impact these services have on children, families, and society as a whole (Buchholz, Burnett, Margolis, Millar, & Talmi, 2018; Heckman, 2011).
Medical settings provide an excellent opportunity to reach young children and their families early and often, thus increasing access to mental health care that is accessible. Infusing infant and early childhood mental health (IECMH) into medical settings is an important strategy to increase access to mental health care and to take a family-centered, multi-generational approach to supporting the health and well-being of young children and their families. Indeed, we believe that when clinical practitioners and policymakers leverage medical settings as essential partners, improved services for infants, toddlers, and their families are seen. What follows are examples of just that—various efforts to permeate medical settings, and policies and procedures relevant to young children seen in medical settings, with a pervasive IECMH lens.
The subsequent sections describe work done within academic medical settings on behalf of infants, toddlers, and families. As members of the 2018–2020 ZERO TO THREE Fellowship class, we spent a significant amount of time considering our role in supporting the infusion of maternal, infant, and early childhood mental health in various medical settings including opportunities for leadership and advocacy. Jennifer Harman describes efforts to better support infants and toddlers with cancer and their families, Melissa Buchholz discusses the expansion of HealthySteps in the state of Colorado, and Obianuju O. Berry explains collaboration between advocacy organizations and medical settings in response to intimate partner violence. Each section begins with background contextual information to help orient the reader.
Cancer in Infancy and Early Childhood—Jennifer Harman
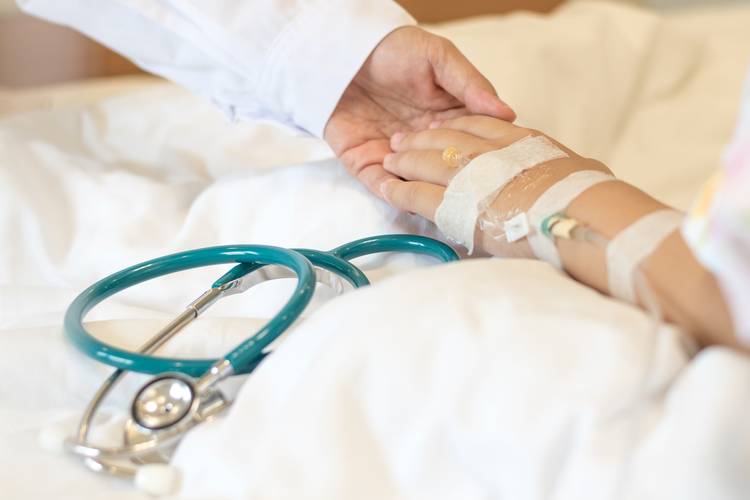
The early environments to which infants and toddlers are exposed matter greatly, and nurturing relationships are essential to the promotion of healthy growth and development of all children, including those battling pediatric cancer. Although childhood cancer continues to be relatively rare, approximately half of all invasive pediatric cancer occurs during the early childhood years, with the highest incidence occurring among babies less than 12 months old (U.S. Cancer Statistics Working Group, 2017). Unfortunately, infants and toddlers who receive treatment for childhood cancer miss common developmental exposures known to aid in sustaining caregiver and infant well-being (Harman, Wise, & Willard, 2018). For example, parents of an infant who is hooked up to intravenous lines might avoid having their child engage in tummy time for fear it might tangle the lines or hurt the baby; yet, this avoidance interrupts activities known to promote development. Similarly, a baby with severe chemotherapy-induced mucositis who is unable to breastfeed or bottle-feed might be considered medically fragile. The parents who believe the infant is medically fragile might avoid holding their baby during enteral feeding, or be encouraged by well-meaning but ill-informed staff to avoid holding their baby during feeding, thus missing natural opportunities to promote secure attachment and interrupting occasions to engage in various “serve-and-return” interactions. Regrettably, situations such as this occur when pediatric oncology care providers are not well versed in the science of early childhood, in general, and factors known to impact overall well-being in infancy, more specifically.
While many institutions that treat infants and toddlers with cancer offer psychosocial care (Wiener, Kazak, Noll, Patenaude, & Kupst, 2015) these services commonly are described as uncoordinated, inconsistent, and indiscriminate (Jones et al., 2018; Scialla et al., 2018), which is much of the antithesis of what would be considered best practice according to IECMH principles. In addition, my professional experience when collaborating with colleagues across institutions highlights a general lack of knowledge among many pediatric oncology psychosocial and medical care providers regarding what IECMH is. Which begs the question, if providers do not know what IECMH is, how can they be expected to infuse its principles or characteristics into their care?
Although many in the pediatric oncology world are new to the concept of IECMH, the pediatric oncology literature illuminates the particular vulnerability of brain development early in life (e.g., Jacola et al., 2016). Indeed, pediatric oncology research clearly supports the need to intervene early in efforts to promote the overall well-being and development of these young children. For example, some pediatric cancers and associated treatments are linked to social and cognitive late effects, meaning that many young children who are successfully treated for cancer are at increased risk for impaired learning, memory weaknesses, and difficulties with executive and social functioning years after completion of cancer-directed treatment (Bornstein et al., 2012; Cox et al., 2019; Kenney, Harman, Molnar, Jurbergs, & Willard, 2019; Willard et al., 2014; Willard et al., 2017), with younger age at time of diagnosis and treatment consistently associated with significantly poorer outcomes (Jacola et al., 2016). This age-based risk factor, while likely unsurprising to those who specialize in work with young children and their families, is particularly concerning given the overrepresentation of very young children among new cases of invasive pediatric cancer.
Armed with the aforementioned knowledge, several steps have been taken to advocate for babies and toddlers in the pediatric oncology world. For example, researchers presented information about cognitive and social late effects to policymakers in Tennessee, resulting in various pediatric cancer diagnoses automatically qualifying young children with cancer histories for early intervention services in that state (Parris, Harman, Jurbergs, Allen, & Canavera, 2019). In other words, in the state of Tennessee a young child now qualifies for early intervention’s supportive services before evidence of cognitive and social late effects emerges.
As another effort to help young children with cancer, staff at St. Jude Children’s Research Hospital initiated an interdisciplinary clinic grounded in IECMH principles. This clinic, St. Jude’s Early Childhood Clinic, conducts developmental assessments with young children with cancer; it systematically provides them and their families with critical prevention and early intervention services, including, but not limited to, relationship-based dyadic therapy, while the young child undergoes medical treatment; and, it assists these families with accessing similar appropriate, interdisciplinary, family-centered services upon return to their home communities. Initiation of St. Jude’s Early Childhood Clinic resulted in more than a 600% increase per year in the number of young children receiving IECMH–informed interdisciplinary prevention and intervention services at this institution.
Although the efforts described thus far serve young children with cancer from Tennessee and those at one hospital well, many children with cancer are treated at institutions other than St. Jude. One effort to reach all families of young children with cancer capitalizes on the Together, Powered by St. Jude Children’s Research Hospital (Together) website (St. Jude Children’s Research Hospital, n.d.-a). This website provides a wealth of accurate, easily digestible, relevant information to families affected by childhood cancer. It is a comprehensive, free online resource. The Together website was expanded to include sections devoted specifically to topics germane to infants and toddlers with cancer and tailored to families of very young children with cancer (St Jude Children’s Research Hospital, n.d.-b). This expansion is a good start. Yet, it is imperative that plans for continued growth of this resource are seen through fruition. Further inclusion of additional ways to foster resilience, to strengthen relationships, to promote ongoing development in the face of a catastrophic diagnosis, and to do so while honoring and celebrating young children and families’ diversity and individual differences is not only slated but it also is critical to the promotion of IECMH within the pediatric oncology world.
HealthySteps/Early Childhood Integrated Behavioral Health—Melissa Buchholz
Most young children will never encounter the adversities associated with undergoing pediatric cancer treatment at a young age; however, an overwhelming majority of infants and toddlers will be seen in medical settings several times before they are 3 years old. Certainly, primary care settings offer ample opportunity for providing mental health services in a setting that is almost universally accessed by young children and their families. The medical home model calls for primary care settings to provide care that is individualized, strengths-based, culturally sensitive, accessible, comprehensive, and family-centered (Stille et al., 2010). In order to accomplish these lofty goals, primary care settings must take a relationship-based approach to providing medical care to children, focusing on whole-child and whole-family care. Young children show up in primary care offices frequently (a recommended 11 times in the first 3 years of life), making this setting well-suited to prevent mental health concerns by promoting healthy development and the importance of early relationships.

Medical settings provide an excellent opportunity to reach young children and their families early and often, thus increasing access to mental health care that is accessible. Photo: Lordn/shutterstock
Although primary care settings are well-positioned to provide this type of care, it can be challenging for integrated clinicians to be intentional about attending to the needs of young children. While integrated behavioral health in primary care has gained traction as a valuable approach to meeting the mental and behavioral health needs of children (Kazak, Nash, Hiroto, & Kaslow, 2017), the focus has not traditionally been on prevention and health promotion strategies but rather on identifying and treating mental health diagnoses and managing crises (e.g., suicidality). The fee-for-service landscape of the health care system also creates challenges for providing services that are preventative in nature. Practices benefit from having a clear and specific mechanism or strategy for delivering this type of care to young children.
HealthySteps is an evidence-based model for delivering integrated early childhood behavioral health services in pediatric primary care settings. The model embeds a professional with expertise in early childhood mental health and development into a primary care setting, resulting in a transformation of the primary care practice to be intentional about supporting their young patients (from birth to 3 years old). The model takes a tiered approach to care for children— including providing universal screening processes, brief developmental and behavioral consultations with families, and, at the highest level of care, team-based well-child visits for children and families deemed at highest risk. The outcomes of HealthySteps have shown that children are more likely to receive well-child visits and vaccinations on time and less likely to visit the emergency room (Guyer, et al., 2003), increases in positive parenting practices (Caughy, Huang, Miller, & Genevro, 2004), and widens the scope of what families discuss during their primary care visits (Buchholz & Talmi, 2012) to name a few.
These very positive and compelling outcomes, the universal approach to providing comprehensive care in primary care, and the relatively low cost of the model have created growing momentum to scale HealthySteps across the country. In Colorado, HealthySteps has gained support from both state and private partners and has grown from three sites implementing the model to 15 sites across the state. There is a desire to see the model grow even further across the state. Leaders of HealthySteps in Colorado are working to support equitable access to behavioral health, particularly prevention and health-promotion strategies, for young children and their families in the state. However, the process of moving this vision forward cannot happen without partners, perspective, perseverance, and public will.
Several important strategies have been vital to the work of growing and sustaining HealthySteps. Having a close and collaborative relationship with the HealthySteps National office at ZERO TO THREE is essential. The National Office shares the goal of scaling and sustaining the model. They are an invaluable partner to providing fidelity guidance and model expertise. In addition, in Colorado, it has been important to have a statewide entity (the State Intermediary Office) leading growth and sustainability efforts. The State Intermediary is a multiagency effort between a nonprofit and Children’s Hospital, and each agency brings unique expertise to the collaboration (strong community partnerships for the former and lengthy implementation and clinical experience for the latter). The nonprofit is positioned to assess community readiness and leverage relationships to advocate for growth, while the hospital provides a setting to maintain implementation and model expertise, pilot quality improvement strategies, and provide on-site training and workforce development. The combination of these important areas of expertise, in addition to close partnership and guidance from the National Office, has been essential to the growth and sustainability efforts across the state.
Forming relationships and cultivating partnerships in diverse sectors have been critical to the effort to scale and sustain HealthySteps. These partners offer unique and informative perspectives about the work and help to promote the advocacy agenda for HealthySteps. Building public will is important, although not sufficient; perseverance in this work is also critical. Setbacks and challenges are to be expected, yet these cannot be seen as roadblocks but rather opportunities to deepen understanding of the systems that impact the vision to grow and sustain the model.
Mental Health Treatment of Intimate Partner Violence Across Systems—Obianuju O. Berry
Just as forming and cultivating relationships are imperative to ensuring better support for infants and toddlers with cancer and to the expansion of HealthySteps in the state of Colorado, they are vital to the response to intimate partner violence (IPV) if one hopes to foster positive environments for children. Indeed, collaboration between disparate services can transform people’s lives. Unfortunately, the fields of advocacy and mental health within IPV have often ignored one another despite the strong bidirectional nature of IPV and mental health disorders. For example, IPV increases the risk of mental health conditions (e.g., post-traumatic stress disorder, depression, anxiety, suicide attempts), which themselves increase the vulnerability to IPV. However, there are concerns that the medical model adopted by mental health services is outdated and fails to acknowledge the role and effect of abuse (Humphreys & Thiara, 2003), meet survivor’s complex needs (Simmel, Postmus, & Lee, 2016), and pathologizes IPV-related difficulties (Tsai, Tomlinson, Comulada, & Rotheram-Borus, 2016).
For women who are mothers, this situation is especially complex, because children who are exposed to IPV experience harm from witnessing the abuse as well as from parenting that is compromised. Caregivers who develop adverse mental health outcomes from IPV are even more at risk for poor parenting skills. For example, maternal depression has been found to negatively impact maternal self-efficacy (i.e., a mother’s ability to be sensitive and responsive to a child; Kohlhoff & Barnett, 2013). Young children are especially affected as IPV has a high incidence during the first year postpartum (70%–80%) when at least one incident of IPV is reported during pregnancy (Charles & Perreira, 2007; Martin, Mackie, Kupper, Buescher, & Moracco, 2001). This is confirmed by statistics from the National Survey of Children’s Exposure to Violence, in which it was shown that witnessing a familial assault was one of the most commonly experienced forms of violence during infancy (Hamby, 2011). In addition, 64% of children exposed to IPV initially witnessed this violence in their first year of life (Graham-Bermann & Perkins, 2010). The adverse consequences associated with early IPV exposure set the stage for continued difficulties throughout the developmental lifespan of the child. Yet, children exposed to IPV exhibit quite variable outcomes, and not all exhibit trauma symptoms. In fact, data suggests that protective factors such as supportive parenting can stabilize and offset the ill effects of IPV exposure (Dalton, Drozd, & Wong, 2004). Thus, improving the mental health of parents with IPV histories improves their parenting and ultimately improves the health and overall well-being of children.
Children who are exposed to interpersonal violence experience harm from witnessing the abuse as well as from parenting that is compromised. Photo: Capifrutta/shutterstock
Despite strong evidence for associations between IPV and psychiatric disorders, the social and emotional needs of IPV survivors continue to go unmet. While 85% of IPV survivors who present to advocacy organizations in the United States report at least one mental health problem, only one third have seen a mental health professional during the past year (Family Justice Center Alliance, 2014). This mismatch in supply and demand points to the significant structural and systemic barriers that prevent survivors from accessing mental health care. It is important to note that these obstacles are especially pronounced for minority women, who in the U.S. are less likely than white women to seek help from various formal and informal sources (Lipsky, Caetano, Field, & Larkin, 2006). With improved access and better treatment, costly emergency room visits could be prevented, which is an especially salient point considering that these emergency room visits place a burden on a health care system that is insufficiently equipped to deal with both mental health concerns and IPV-related concerns. Appropriate provisions of services for these survivors would ideally incorporate knowledge of both mental health concerns and IPV-related concerns; yet, few models of such psychiatric service provisions exist (Berry, Okuda Benavides, Weiss, Fitelson, & Monk, 2019).
New York City is tackling this very issue with a tripartite partnership with private, public, and academic collaboration that imbeds skilled mental health clinicians within the Family Justice Center, a resource center for survivors of IPV and sex trafficking. New York boasts the largest network of Family Justice Centers in the country, operated by the Mayor’s Office to End Domestic and Gender Based Violence. This new collaboration, which is the nation’s first such integrated mental health model, provides free, evidence-based treatment, including psychotherapy, skills-based learning, and psychopharmacology in a trauma- and culturally informed capacity. By bringing experienced mental health clinicians to the community, the program is meeting the survivors where they are, and where they feel the safest. Not only do the survivors continue to report feeling safe physically, but they also report feeling safe emotionally with this added resource. Even more impactful are the changes in their interpersonal relationships. Of the survivors who received mental health services, 92% of them reported improvement in their parenting relationships with their children (Berry & Fitelson, 2019).
The enormity of IPV consequences, including mental health and compromised parenting, affects everyone and requires integrated services to help communities heal. Mental health supports for caregivers are resources that help foster those supportive relationships and positive environments for children. Communities must invest in collaborative systems across disciplines to ensure that all people can get the treatment they need regardless of the barriers in their way.
Conclusion
Many who work within medical settings face and overcome obstacles in efforts to integrate collaborative supports for young children and families. Indeed, we are only a few of the many working to promote IECMH through our positions in academic medical systems. Although the preceding examples demonstrate only a fraction of the work being done on behalf of young children and their families in these settings, each example highlights the collaboration, perseverance, and adaptability necessary to make changes for the betterment of infants, toddlers, and their families; and all describe the literal and figurative advantage of meeting families (and systems) where they are.
Each example further illustrates that services need to support the whole child and the whole family in order to promote optimal outcomes for young children. Families deserve access to preventative, non-stigmatized, family-centered mental health services that support the health and well-being of young children. Medical settings and partnerships inclusive of medical settings offer the opportune context for such efforts.
Author Bios
Jennifer Harman, PhD, is a pediatric psychologist faculty member at St. Jude Children’s Research Hospital. Dr. Harman holds a bachelor’s degree in psychology from the University of Memphis and master’s and doctoral degrees in school psychology with specialization in early childhood from the University of Florida. She completed her clinical doctoral internship and her postdoctoral fellowship at the Yale University Child Study Center. Dr. Harman joined the clinical staff at St. Jude Children’s Research Hospital in 2011 as a staff psychologist; and she joined the clinical faculty as an assistant member in 2018. Dr. Harman co-created an interdisciplinary early childhood clinical service at St. Jude Children’s Research Hospital based upon early intervention expertise, infant mental health principles, and known best practices for working with very young children and their families. She is involved in clinical training and provides direct clinical psychological services to young patients with cancer and/or catastrophic hematological diagnoses and their families. Dr. Harman also remains actively involved in clinical investigation related to the social, emotional, adaptive, and cognitive functioning of young children with cancer or sickle cell disease. She has worked with local and state policymakers to ensure that adequate and appropriate support services are in place for young children with cancer and their families; and she is an invited member of the Tennessee Young Child Wellness Council, a strong statewide early childhood collaboration.
Melissa Buchholz, PsyD, is a licensed clinical psychologist and assistant professor at the University of Colorado School of Medicine in the Harris Program for Child Development and Infant Mental Health. Dr. Buchholz is passionate about disseminating health promotion and prevention activities for young children and has spent her career focusing on integrating early childhood behavioral health services into medical settings, specifically pediatric primary care. Dr. Buchholz is particularly interested in improving access to behavioral health care for young children and building comprehensive systems of care for young children and their families. Dr. Buchholz is the director of HealthySteps for the state of Colorado and has worked to scale this model across the state since 2012. In addition, she provides consultation and technical assistance to assist pediatric practices with expanding behavioral health services to include a focus on young children and their families. She actively advocates for young children and their families locally and nationally.
Obianuju “Uju” O. Berry, MD, MPH, is a graduate of Harvard Medical School, the Johns Hopkins Bloomberg School of Public Health, the NewYork-Presbyterian/Columbia/NYSPI Psychiatry Residency Training Program, and the NewYork-Presbyterian Child and Adolescent Psychiatry Residency Training Program. She has expertise in child/adolescent and adult psychiatry, as well as reproductive psychiatry. Dr. Berry is experienced in mental health research and public policy, and has worked with a variety of state and federal institutions, including the Centers for Disease Control and Prevention, the U.S. Department of Health and Human Services, and the National Institute of Domestic Violence in the African American Community. She currently is leading a city-wide hybrid implementation effectiveness study on the evaluation of the collaboration between psychiatry and intimate partner violence with New York City’s Mayor’s Office to End Domestic and Gender Based Violence (ENDGBV). Dr. Berry’s research and clinical interests include child/adolescent mental health, epidemiology, trauma, service implementation, and working with minority and immigrant populations.
Suggested Citation
Harman, J., Buchholz, M., & Berry, O. B. (2020). Infusing infant and maternal mental health into health care settings. ZERO TO THREE Journal, 40(5), 50–56.
References
Berry, O., & Fitelson, E. (2019). The Family Justice Center mental health collaboration: From concept to practice. New York, NY: Columbia University Medical Center.
Berry, O., Okuda Benavides, M., Weiss, M., Fitelson, E., & Monk, C. (2019). Collaborations between domestic violence psychiatric services: A review of the literature. New York, NY: Columbia University Medical Center.
Bornstein, M. H., Scrimin, S., Putnick, D. L., Capello, F., Haynes, O. M., Falco, S., …Pillon, M. (2012). Neurodevelopmental functioning in very young children undergoing treatment for non-CNS cancer. Journal of Pediatric Psychology, 37, 660–673.
Buchholz, M., Burnett, B., Margolis, K. L., Millar, A., & Talmi, A. (2018). Early childhood behavioral health integration activities and HealthySteps: Sustaining practice, averting costs. Clinical Practice in Pediatric Psychology, 6(2), 140–151.
Buchholz, M., & Talmi, A. (2012). What we talked about at the pediatrician’s office: Exploring differences between HealthySteps and traditional pediatric primary care visits. Infant Mental Health Journal, 33(4), 430–436.
Caughy, M. O., Huang, K., Miller, T., & Genevro, J. L. (2004). The effects of the HealthySteps for Young Children program: Results from observations of parenting and child development. Early Childhood Research Quarterly, 19(4), 611–630.
Charles, P., & Perreira, K. M. (2007). Intimate partner violence during pregnancy and 1-year post-partum. Journal of Family Violence, 22(7), 609–619. doi:10.1007/s10896-007-9112-0
Cox, L. E., Kenney, A. E., Harman, J. L., Jurbergs, N., Molnar, A. E. Jr., Willard, V. W. (2019). Psychosocial functioning in young children treated for cancer: Findings from a clinical sample. Journal of Pediatric Oncology Nursing, 36, 17–23.
Dalton, C., Drozd, L. M., & Wong, F. Q. (2004). Navigating custody and visitation evaluations in cases with domestic violence: A judge’s guide. Reno, NV: National Council of Juvenile and Family Court Judges.
Family Justice Center Alliance. (2014). Health survey report: Addressing health needs of intimate partner violence survivors in Family Justice Center. Retrieved from source
Graham-Bermann, S. A., & Perkins, S. (2010). Effects of early exposure and lifetime exposure to intimate partner violence (IPV) on child adjustment. Violence and Victims, 25(4), 427–439. doi:10.1891/0886-6708.25.4.427
Guyer, B., Barth, M., Bishai, D., Caughy, M., Clark, B., Burkom, D.,… Tang, C. (2003). Healthy Steps: The first three years: The HealthySteps for Young Children Program national valuation. Baltimore, MD: Johns Hopkins Bloomberg School of Public Health.
Hamby, S. L. (2011, October). Children’s exposure to intimate partner violence and other family violence. Juvenile Justice Bulletin (1–11). Retrieved from source
Harman, J. L., Wise, J., & Willard, V. W. (2018). Early intervention for infants and toddlers: Applications for pediatric oncology. Pediatric Blood and Cancer, 65, e26921. doi: 10.1002/pbc.26921
Heckman, J. J. (2011). The economics of inequality: The value of early childhood education. American Educator, 35(1), 31–35.
Humphreys, C., & Thiara, R. (2003). Mental health and domestic violence: “I call it symptoms of abuse.” British Journal of Social Work, 33(2), 209–226. doi:DOI 10.1093/bjsw/33.2.209
Jacola, L. M., Krull, K. R., Pui, C. H., Pei, D., Cheng, C., Reddick, W. E., & Conklin, H. M. (2016). Longitudinal assessment of neurocognitive outcomes in survivors of childhood acute lymphoblastic leukemia treated on a contemporary chemotherapy protocol. Journal of Clinical Oncology, 34, 1239–1247. doi: 10.1200/JCO.2015.64.3205.
Jones, B., Currin-McCulloch, J., Pelletier, W., Sardi-Brown, V., Brown, P., & Wiener, L. (2018). Psychosocial standards of care for children with cancer and their families: A national survey of pediatric oncology social workers. Social Work Health Care, 57(4), 221–249.
Kazak, A. E., Nash, J. M., Hiroto, K., & Kaslow, N. J. (2017). Psychologists in patient-centered medical homes (PCMHs): Roles, evidence, opportunities and challenges. American Psychologist, 72(1), 1–12.
Kenney, A. E., Harman, J. L., Molnar, A. E. Jr, Jurbergs, N., & Willard, V. W. (2019). Early cognitive and adaptive functioning of clinically referred infants and toddlers with cancer. Journal of Clinical Psychology in Medical Settings. Advanced online publication. doi:10.1007/s10880-019-09619-1
Kohlhoff, J., & Barnett, B. (2013). Parenting self-efficacy: Links with maternal depression, infant behaviour and adult attachment. Early Human Development, 89(4), 249–256. doi:10.1016/j.earlhumdev.2013.01.008
Lipsky, S., Caetano, R., Field, C. A., & Larkin, G. L. (2006). The role of intimate partner violence, race, and ethnicity in help-seeking behaviors. Ethnicity & Health 11(1), 81–100. doi:10.1080/13557850500391410
Martin, S. L., Mackie, L., Kupper, L. L., Buescher, P., & Moracco, K. E. (2001). Physical abuse of women before, during, and after pregnancy. Journal of the American Medical Association, 285(12), 1581–1584. doi:DOI 10.1001/jama.285.12.1581
Parris, K. R., Harman, J. L., Jurbergs, N., Allen, J. M., & Canavera, K. E. (2019). Beyond clinical practice in pediatric psychology: Illustrative experiences in influencing practice changes, public opinion, and governmental policies. Psychological Services. Advance online publication. http://dx.doi.org/10.1037/ser0000385
Scialla, M. A., Canter, K. S., Chen, F. F., Kolb, E. A., Sandler, E., Wiener, L., & Kazak, A. E. (2018). Delivery of care consistent with the psychosocial standards in pediatric cancer: Current practices in the United States. Pediatric Blood & Cancer, 65, 1–9.
Simmel, C., Postmus, J. L., & Lee, I. (2016). Revictimized adult women: Perceptions of mental health functioning and associated services. Journal of Family Violence, 31(6), 679–688. doi:10.1007/s10896-015-9796-5
Stille, C., Turchi, R. M., Antonelli, R., Cabana, M. D., Cheng, T. L., Laraque, D., Perrin, J., & Academic Pediatric Association Task Force on Family-Centered Medical Home. (2010). The family-centered medical home: Specific considerations for child health research and policy. Academic Pediatrics, 10(4), 211–217
St. Jude Children’s Research Hospital. (n.d.-a). How cancer may affect early childhood development. Retrieved from source
St. Jude’s Children’s Research Hospital. (n.d.-b). Your home base to face cancer. Retrieved from source
Tsai, A. C., Tomlinson, M., Comulada, W. S., & Rotheram-Borus, M. J. (2016). Intimate partner violence and depression symptom severity among South African Women during pregnancy and postpartum: Population-based prospective cohort study. PLOS Medicine, 13(1). doi:ARTN e100194310.1371/journal.pmed.1001943
U. S. Cancer Statistics Working Group. (2017). United States cancer statistics: 1999–2014 incidence and mortality web-based report. Atlanta, GA: U. S. Department of Health and Human Services, Centers for Disease Control and Prevention, and National Cancer Institute. Retrieved from source
Wiener, L., Kazak, A. E., Noll, R. B., Patenaude, A. F., & Kupst, M. J. (2015). Standards for the psychosocial care of children with cancer and their families: An introduction to the special issue. Pediatric Blood & Cancer, 62, S419–S424.
Willard, V. W., Cox, L. E., Russell, K. M., Kenney, A., Jurbergs, N., Molnar, A. E., & Harman, J. L. (2017). Cognitive and psychosocial functioning of preschoolage children with cancer. Journal of Developmental & Behavioral Pediatrics, 38, 638–645.
Willard, V. W., Qaddoumi, I., Chen, S., Zhang, H., Brennan, R., Rodriguez-Galindo…Phipps, S. (2014). Developmental and adaptive functioning in children with retinoblastoma: A longitudinal investigation. Journal of Clinical Oncology, 32(25), 2788–2793.