
University of Minnesota’s Birth to Three Clinic: Comprehensive Assessment and Diagnosis Across Diverse Settings

Abstract
The University of Minnesota’s Birth to Three Clinic has adopted a holistic approach to supporting children’s needs within an attachment-focused, trauma-informed, and neurodevelopmental framework rooted in the DC:0–5TM classification framework. This clinical framework of infant and early childhood mental health (IECMH) assessment has been applied in two settings: (1) a pediatric inpatient intensive care unit (PICU) working with medically complex young children and (2) a multidisciplinary outpatient clinic for children in the foster care system or post-adoption. In both settings, our work is focused on young children who have experienced a variety of early life stressors and adversity.
In recent decades, the understanding of the complexities underlying variation in development trajectories has been propelled by the academic field of developmental psychopathology. Advances in basic and translational science have yielded complex theoretical models and a more nuanced conceptualization of children’s vulnerability to their environment, the importance of primary caregivers, and the capacity for resilience in the first years of life. Nevertheless, bridging scientific advancements and clinical practice within the field of infant and early childhood mental health (IECMH) remains an important area for future growth. While still limited, IECMH clinics and programs have become more available in recent years. Yet, even with the increased access to IECMH services, comprehensive assessment and diagnosis of young children still lags behind the research literature. More specifically, there is a need for systematic implementation of IECMH assessment that goes beyond clinical diagnosis, and simultaneously holds the child, the parent(s), their relationships, and the broader environment/social context in mind.
Despite understanding the complexities of early brain and social–emotional development, many young children are still diagnosed under a single axial system, in line with approaches to mental health diagnosis among older children, adolescents, and adults. The DC:0–5TM: Diagnostic Classification of Mental Health and Developmental Disorders of Infancy and Early Childhood, Version 2.0 (DC:0–5; ZERO TO THREE, 2021) provides an exception to this single axial system, outlining diagnostic criteria and important cultural, developmental, and other contextual considerations affiliated with mental health diagnoses for young children from birth to 5 years old. Decades of research have underscored the impact of multilevel systems and their interactions on child development, which is reflected in the DC:0–5 diagnostic framework. More specifically, it is critical to acknowledge the unique vulnerability of young children to external factors and the importance of considering early brain development in the context of relationships; not attending to these key components does a disservice to the assessment process, diagnostic process, case conceptualization, clinical practice, and intervention planning. The DC:0–5 diagnostic classification system provides a framework for clinicians to consider the complexities of early childhood when determining an appropriate diagnosis and when formulating clinical recommendations and subsequent treatment.

The current edition of the DC:0–5 classification system utilizes five separate axes:
- Axis I includes relevant clinical diagnoses (e.g., neurodevelopmental disorders, anxiety-related disorders);
- Axis II assesses the relational context (i.e., quality of the caregiver–child relationship and caregiving environment);
- Axis III covers comorbid physical health conditions and considerations (e.g., chronic medical conditions, previous medical procedures);
- Axis IV acknowledges current psychosocial stressors (e.g., economic stressors, limited social support); and
- Axis V provides a brief assessment of the child’s current developmental competence across emotional, social– relational, language/social communication, motor/ physical, and cognitive domains (ZERO TO THREE, 2021).
With attention to these complex and interacting factors, the DC:0–5 multiaxial approach to diagnosis provides a way of organizing data from full developmental assessments in outpatient mental health clinics and integrative, behavioral health care programs that embed IECMH services into existing medical care. The assessment battery, which includes multiple forms of information in conjunction with the DC:0–5 classification framework, allows for identification of specific infant and young childhood disorders. It is important to note that DC:0–5 is a diagnostic classification system and is not a screening or an assessment tool (see Box 1).
Box 1. Defining Assessment and Diagnosis
The DC:0–5 manual provides the following definitions:
Assessment is the result of gathering information from review of records, obtaining history from caregivers, and conducting informal and more structured observations of behavior…The assessment process is ongoing…one collects information about the infant/young child’s behavior over time…
Diagnosis is the identification and classification of specific infant/ young child disorders. The primary purpose of the classification of disorders is so that professionals can communicate clearly about descriptive syndromes…using the common language of a diagnostic classification system facilitates the connection of individuals to existing services and can thus aid in the mobilization of appropriate systems of mental health care. (ZERO TO THREE, 2021, pp. 6–7)
The Birth to Three Clinic
Conceptualizing the many ecological and relational factors that impact children’s physical and mental health is of particular importance when working with young children who have complex histories and presenting concerns, including various forms of early life trauma and adversity. To meet this need, the Birth to Three Clinic and Early Childhood Mental Health Program (BTT Clinic) was established in 2015 within the University of Minnesota Department of Pediatrics. This clinic specializes in comprehensive IECMH assessment and treatment services for children from birth to 3 years old, with an emphasis on supporting children experiencing various complexities: comorbid medical conditions, prolonged hospitalizations, prenatal exposures (e.g., drugs, alcohol, or other teratogen), international or domestic adoption, and/or involvement in the foster care system. In the context of a large, metropolitan, academic medical center, the BTT Clinic incorporates important principles from clinical practice and developmental research. By understanding the literature on early childhood brain development, developmental psychopathology, and risk and resilience factors within the parent–child relationship, the BTT Clinic takes a holistic approach to supporting children’s needs within an attachment- focused, trauma-informed, and neurodevelopmental framework. Early in the clinic’s inception, providers on the BTT clinical team advocated for training in and use of the DC:0–5 diagnostic framework.
We previously published information about the BTT Clinic’s use of the DC:0–5 diagnostic system, outpatient assessment protocol, and adaptions within certain specialty populations (Dahl et al., 2023). In the current article, we will further elaborate on how this same clinical framework and approach to IECMH assessment can be applied in two settings: (1) in a pediatric inpatient intensive care unit (PICU) working with medically complex young children and (2) in a multidisciplinary outpatient clinic for children in the foster care system or post-adoption. Though the contexts of our programs differ, the common thread is our work with young children who have experienced a variety of early life stressors and in many cases different forms of trauma. We chose to focus on young children because they are in a critical window of brain development, wherein the appropriate supports and interventions can optimize healing and their developmental trajectory.
Pediatric Intensive Care
According to the American Academy of Pediatrics, approximately 92% of all American children under 2 years old visited office-based physicians (American Academy of Pediatrics, 2022), placing the medical system in a unique position to identify early developmental and mental health concerns and make referrals for further assessment or intervention. Nevertheless, there is a gap between this noted opportunity for early identification in pediatric settings and the implementation of mental health training and supportive programs (Osofsky & Lieberman, 2011; Shonkoff et al., 2012), particularly for children from birth to 5 years old. In general, IECMH concerns tend to go unidentified in pediatric contexts, perhaps due to a lack of training in early risk factors and limited understanding of the manifestation of mental health symptoms in the first few years of life. For example, medical providers may underestimate the psychological and developmental impact of early medical trauma. Identification can be particularly difficult in PICU settings, where the primary focus is often on the physical health and survival of young patients. And yet, young children in the hospital—and particularly those with complex, chronic medical conditions— have the potential to experience toxic stress when they encounter stressful medical events without adequate relational buffering or co-regulation.
Young children who are hospitalized in the PICU are at unique risk for negative mental health outcomes secondary to congenital or chronic health conditions, which alter the course of development at the level of the child and the family system. Chronic illness can cause repeated exposure to stressful events such as multiple surgeries, hospitalizations, medical visits, and blood draws. In cases when these medically compromised children also lack a consistent and supportive caregiving relationship, each of these exposures to a stressful event has the potential to become “toxic,” further rewiring brain networks, altering the stress response system, and placing these medically fragile children at an even greater risk for long-term negative outcomes.
One specific group that is at particularly high risk for IECMHchallenges is children with critical congenital heart disease (cCHD). With medical advances, more than 97% of newborns with congenital heart disease survive to adulthood (Mandalenakis et al., 2020). Those with cCHD are the most fragile subset, and these patients face significant medical morbidity and mortality. This medical complexity often leads to prolonged hospitalizations in the PICU and can be associated with significant social–emotional adversity. Thus, there is a critical need for IECMH services and multiaxial approaches to diagnosis among this high-risk group of children in order to proactively identify areas of concern and follow up with targeted evidence-based interventions, rather than waiting to reactively treat mental health conditions later in development.

Piloting the PICU Model
The BTT Clinic currently provides inpatient-based IECMH assessment services to all pediatric patients from birth to 3 years old who have been hospitalized on the cardiovascular pediatric intensive care unit (CV-PICU) for 2 weeks or more. Hospitalization length was chosen as the inclusion criteria because prolonged hospitalization often implies medical complexity and enhanced risk factors that may impact a child’s developmental trajectory. The CV-PICU assessment protocol consists of four distinct parts, which support DC:0–5 diagnoses and inform a more comprehensive understanding of the child, the parent–child relationship, and the broader contextual environment. We briefly describe the four components of this assessment approach in the following sections, indicating ways in which our approach informs different axes within the DC:0–5 framework.
Chart Review
First, a chart review is conducted with a focus on early childhood stressors that may be impacting the child’s physical, social–emotional, and developmental capacity, such as surgery, medical complexity, and prolonged separations from caregivers. During this chart review, special note is taken of any documentation from social work providers, who are uniquely trained in interacting with families and caregivers, and who may help consult with the BTT Clinic team to better understand the current needs of the family. Information from the initial chart review helps support the team’s understanding of several axes within the DC:0–5 classification system, but most notably informs Axis III (physical health conditions and considerations) and Axis IV (psychosocial stressors).

Caregiver Interviews
Second, interviews are conducted with the child’s caregiver(s) and medical providers, including physicians, nurses, occupational therapists, and respiratory therapists. The interviews focus on the strengths of the child, the caregivers, their relationship, and their responses to stressors. With parents or other caregivers, an adapted version of the Working Model of the Child Interview (WMCI; Zeanah et al., 1997) is implemented to better understand parental representations. Specifically, we modified questions from the WMCI to account for and maintain sensitivity to differences in early life experiences common in cCHD children, such as prolonged hospitalizations, limited ability of parents and caregivers to physically hold their children, and varying levels of medical sedation that may impact the child’s ability to cue and interact with their parents and caregivers. Overall, the general interview and WMCI questions support our understanding of Axis I (clinical diagnoses), Axis II (relational context) and Axis V (developmental competence). Interviews with the medical team may also supplement our understanding of Axis III (physical health conditions and considerations).
Observation
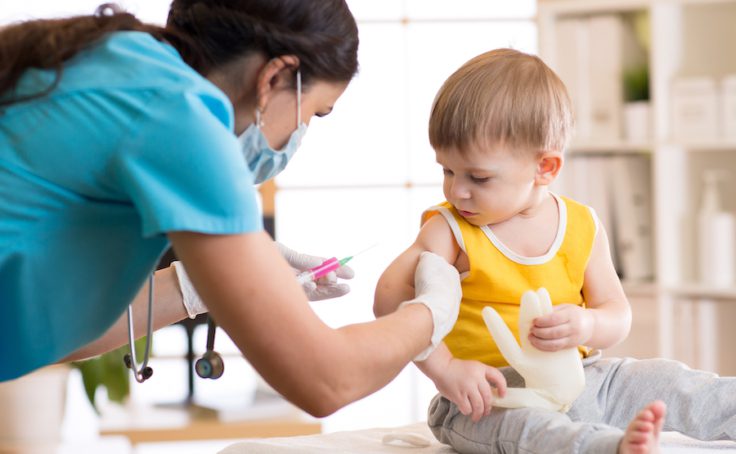
To further support our understanding of Axis I (clinical diagnoses) and Axis II (relational context), the third component of our assessment involves use of an observation protocol based on an adapted version of the Massie-Campbell Scale of Mother Infant Attachment (Massie & Campbell, 1983). The Massie-Campbell Scale of Mother Infant Attachment was originally designed for use with children from birth to 18 months old during a mildly stressful situation. The Massie- Campbell Scale of Mother Infant Attachment focuses on both the young child’s reaction to the stressful event and their caregiver’s response to the child’s stress. In the CV-PICU, stressful events emerge at high frequency, and our team can observe the parent and child through naturally occurring circumstances such as diaper changes, transferring the child from their bed, or a needle stick. Behaviors are rated on a 5-point scale and provide an indication about the synchrony between the child with cCHD and their caregiver. For example, in an inpatient setting, a parent’s response to their child undergoing a needle stick can influence how the child responds to the medical procedure. On one hand, a parent may either gravitate toward their child’s bedside during a medical procedure, to soothe and comfort them using touch (e.g., stroking their head) or verbally (e.g., “It is all going to be okay.”). In this case, the child’s stress from the medical procedure is buffered by their parent. On the other hand, a parent may step back, away from the bed, and let the provider interact with the child. In such a case, the child is left to manage the stress and associated feelings on their own, without the support of their primary caregiver.
Reflective Feedback
The fourth and final component of our adapted IECMH assessment and use of DC:0–5 framework within the CV-PICU is the opportunity for a reflective feedback session with the caregivers. At the end of the assessment process, the BTT clinical team provides a feedback session that emphasizes strengths of the parent(s)/caregiver(s) and child, and we provide brief psychoeducation on child development, stress, and how the caregiver can help buffer stressful experiences the child may encounter while inpatient and postdischarge. As an extension of these four components that occur while the cCHD child is hospitalized on the PICU, every patient who participates in the assessment process is offered a follow-up consult approximately 1 month postdischarge, at which time additional clinical services and other developmental supports may be recommended.
Overall, the goal of this four-component inpatient IECMH assessment, using the DC:0–5 framework as a guide for organizing information, is to help increase parental reflective functioning and parental understanding of their child, especially in the context of ongoing medical care that may be stressful and overwhelming. By using the multiaxial diagnostic approach within a high-risk medical population, we aim to clarify important contextual, cultural, relational, developmental, and physical health factors that may impact the child’s social–emotional well-being. Ultimately, by acknowledging these interacting factors, our goal is to help parents see and support their child in the midst of significant stress. Given the often interacting and multifactorial stressors impacting these children, it is critical to engage with and support these families as early as possible.
Foster Care and Adopted Children
Children with a history of caregiving disruptions or transitions often present with developmental delays and mental health concerns secondary to a number of typically co-occurring factors, such as prenatal exposures to alcohol or other substances, limited access to prenatal care, or postnatal traumatic experiences such as neglect or abuse (Leslie et al., 2002; Pears & Fisher, 2005). Among foster care and adopted children, instability and transitions in child placement are related to an array of emotional and developmental difficulties (Fisher et al., 2016). Multiple transitions in housing (due to caregiver transitions) also create barriers to timely IECMH assessment and the provision of evidence-based services, as children may experience changes in caregivers, case workers, early childhood education/school settings, and the city, county, or state in which they are living, among other transitions. Large numbers of children with early relational adversity or disrupted caregiving do not receive early intervention services (Hartinger-Saunders et al., 2019), placing them at higher risk for possible misdiagnosis of behavioral or conduct disorders later in childhood.
Neurodevelopmental Differences
Young children with medical complexity and/or a neurodevelopmental disability and who are placed in foster care may experience additional social–emotional risk factors and stressors compared to young children without such diagnoses. Platt and Gephart (2022) completed a quantitative descriptive study which analyzed a data set from the Adoption and Foster Care Analysis and Reporting System (commonly known as AFCARS), that comprised 680,611 children in foster care. The researchers found that foster children with medical or disability diagnoses experienced a mean of 4.0 disruptions (e.g., transitions to new homes), compared to 2.37 disruptions for children without a documented medical or disability diagnosis. In addition, foster children with a disability on average spent 915 days in foster care, compared to 514 days for children without a disability.
In the context of IECMH assessment and diagnosis, however, a thorough understanding of brain development is necessary but not sufficient. Using the DC:0–5 approach to diagnosis as a guide, clinicians must seek to understand the whole child within their environment. Decades of research have shown that sensitive and responsive caregiver–child relationships are critical to supporting early brain development, as children develop within the context of these relationships. Early interventions, therefore, require simultaneous consideration of the child’s history, symptoms, and developmental capacity in conjunction with a focus on fostering developmental, relational, and trauma-informed supports. Without adequate buffering of high-risk early adverse experiences by supportive caregivers, the child’s developmental trajectory may be further impacted (Lieberman, 2004). In this way, although their early experiences of adversity and stress may be different, both young children with cCHD and those with a history of caregiving disruptions need approaches to mental health care that involve their caregivers, focus on the parent–child relationship as a mechanism for healing, and consider their symptoms and needs in the context of their broader environment.
Piloting the Integrated Model for Foster Care and Adopted Children
Within the University of Minnesota BTT Clinic, we are currently piloting a model of IECMH assessment and applying the DC:0–5 framework with children who have experienced caregiving disruptions due to placement in foster care or adoption. Anecdotally, we have found a strong need for this within the Adoption Medicine clinic at the University of Minnesota which serves both domestically and internationally adopted children but also children in foster care and their caregivers. To meet the immediate needs of young children who may experience multiple transitions, we designed the integrated model for assessment which helps provide critical information and recommendations quickly. The overarching goal of integrating relational assessments with developmental testing is to “fast-track” access to targeted services and to help support the emerging parent–child relationship. This fast-track protocol consists of three components: (1) initial interview and observations by mental health professionals during an integrated, multidisciplinary medical appointment, and screening for current emotional, behavioral, and traumarelated symptomology; (2) in-clinic developmental and observational assessment using standardized instruments and observational protocols; and (3) reflective feedback and discussion to support the caregiver’s understanding of the child and treatment recommendations.
Interview and Observations
The first component of the fast-track developmental testing model occurs within the Adoption Medicine Clinic at the University of Minnesota. In accordance with the rapid brain development that occurs within the first years of life, our fast-track integrated care approach to IECMH assessment prioritizes children 2.5 years old or younger, who are currently in foster care or adopted, and who have not previously received developmental testing. Within the context of this multidisciplinary medical appointment, our BTT clinical team gathers relevant history, symptoms, developmental concerns, and relational observations. Coordination with our physician and occupational therapy colleagues also helps inform our understanding of the child’s physical health, motor skills, and sensory needs. During this visit, our BTT clinicians observe the child’s behavior in the context of the medical and occupational therapy exams. The broad function of this observation is to aid in our understanding of how the child signals or cues the caregiver, especially during times of stress; the caregiver’s capacity to be a co-regulating partner for the child; the child’s ability to be soothed by their caregiver; and whether the child displays any indiscriminate friendliness with unfamiliar providers (Palmer et al., 2021). This observation can inform multiple DC:0–5 axes, specifically the parent–child relationship as well as developmental capacities.

In this initial visit, parents and caregivers are provided mental health and behavioral screeners about their child that address emotionality, trauma experiences, and current service utilization. Screeners provided include a Baby Pediatric Symptom Checklist for children ages 1 month to 1.5 years old (Sheldrick et al., 2013), the Brief Early Childhood Screening Assessment for children 1.5 to 2.5 years old (Fallucco et al., 2017), and the Child and Adolescent Trauma Screen (Sachser et al., 2017). These screening questionnaires inform our clinical understanding of the child’s early adverse experiences, provide a snapshot of the caregiver’s experience of the child, and provide context to the child’s current presentation. In addition, these screening questionnaires contribute to a more refined understanding of all axes within the DC:0–5 framework.
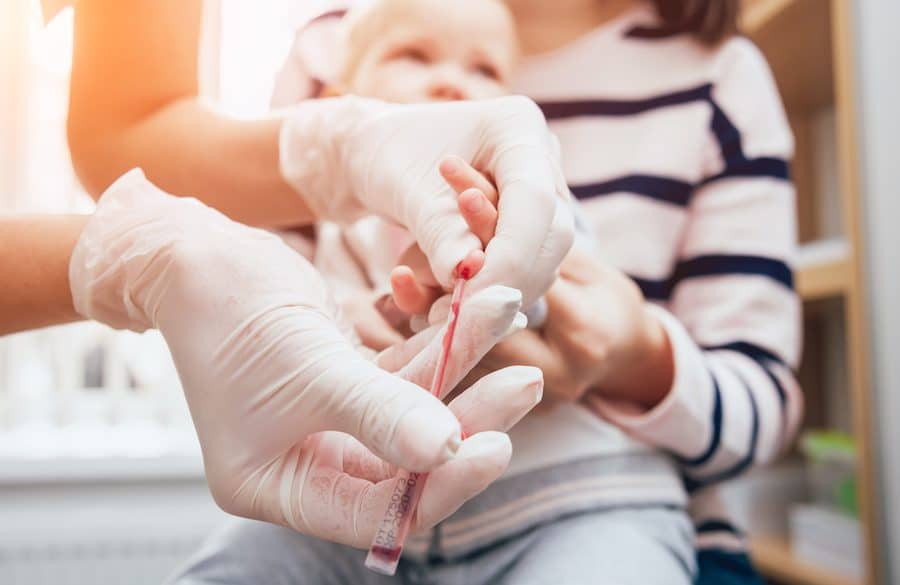
Finally, during this initial interview, opportunities for further observation during the initial Adoption Medicine Clinic visit arise during the medically recommended blood collection, which is used to screen for an array of transmittable diseases. During the blood draw, BTT clinicians have unique insight into the child’s behavior and the caregiver–child relationship status during an increasingly stressful circumstance. For example, we can observe how caregivers are structuring this stressful experience, providing guidance, and offering comfort, even when the child’s signals may be unclear or confusing. BTT clinicians can offer in-vivo comments about child behaviors and reactions and can further reflect with caregivers about how their own emotions and behaviors may impact their children. Again, these observations inform relational contexts and developmental competence of the children.
Developmental Evaluations
The second component of the fast-track model with our mental health team is comprised of behavioral and relationship observations, reflective feedback opportunities, as well as the administration of developmental assessment(s). Developmental assessment provides the opportunity for continued observation as well as information on cognitive development; it is an additional data point in our comprehensive assessment process. We find that offering developmental assessment for these highest- risk children also supports the caregivers, insofar as it offers a more comprehensive understanding of their child’s current capacity and may be particularly validating for caregivers presenting with developmental concerns about their child.
Prior to the second appointment, caregivers fill out the Vineland Comprehensive Parent-Caregiver Form (Sparrow & Cicchetti, 1989). The Vineland provides information on domains including communication, daily living skills, socialization, motor skills, and maladaptive behavior. For children in the designated age range, additional information on emotional and behavioral symptoms is provided through parental responses to a Child Behavior Checklist (Achenbach, 1999) for children between 1.5 and 5 years old. This checklist focuses on behavioral and emotional challenges and competencies. Finally, developmental testing is completed using the Mullen Scales of Early Learning (Mullen, 1995). Although the focus of this appointment is on standardized administration of the developmental testing, we have found that further observation of the child–parent relationship can also be completed in this context. More specifically, the testing environment presents a mild stressor for the child (e.g., unfamiliar setting, demands of testing items). In addition, caregivers may also experience stress and anxiety about testing outcomes, or when explicitly instructed not to assist the child in testing tasks. In this way, unique clinical observations can be made relevant to the child’s frustration tolerance, fatigue, and response to praise, as well as the parent’s capacity to be emotionally present and supportive of the child, even when instructed not to concretely help them complete activities or answer questions. As we observe the caregiver–child relationship during developmental testing, and we can reflect with caregivers in real-time about what their child is experiencing and about their own thoughts and feelings elicited by the testing process. In this way, the developmental assessment experience in and of itself can foster a therapeutic environment that promotes parental reflective functioning and their understanding of their child, in addition to informing the developmental competence axis within the DC:0–5 framework.
Reflective Feedback
The third and final component of the fast-track model includes a reflective feedback session that incorporates data from the initial Adoption Medicine Clinic visit, standardized parent-report questionnaires, behavioral observations, and developmental assessment results. As mentioned, these components collectively inform the multiaxial DC:0–5 diagnosis, helping support a comprehensive conceptualization of the child. Whenever possible, this discussion occurs on the same day postassessment, and reflective questions are incorporated to help parents see their child’s needs and understand recommendations for clinical services.
Conclusion
The development and implementation of both the CV-PICU Assessment Program, as well as the Fast Track Foster Care Integrated Neurodevelopmental Assessment and Early Childhood Mental Health framework, highlight two ways the DC:0–5 framework can be applied across settings with young children. The emphasis on the young child within their specific context and relationships is an important thread in both the inpatient CV-PICU and Adoption Medicine Clinic. Two primary goals of both programs are to accurately assess a young child’s strengths and areas of challenge and to provide parents, caregivers, and providers psychoeducation, support, and a reflective space to process their experiences.
DC:0–5 is a listing of clinical disorders and contextual classifications that assists clinicians in organizing data to inform diagnosis. The framework informs how clinicians conceptualize children and subsequent interventions and supports. It allows for a systematic way of measuring risk factors and current levels of functioning, which in turn allows for more targeted and individualized interventions which can impact outcomes. In addition, using this systematic approach to diagnosis allows for higher quality training of students in our clinic, thus creating a new generation of researchers and clinicians who are well versed in relational and developmental frameworks. Finally, we believe that an integrated approach—including chart review, caregiver interviews, developmental screening and evaluation, observation, and reflective feedback—allows for a diagnostic approach that can be implemented across contexts, wherever there are young children who have experienced early life stressors.
Acknowledgments
Funding for this research was provided through the Minnesota Department of Human Services’ Permanency Support Services Grant.
Quannah Parker-McGowan, PhD, BCBA, is currently an advanced practicum student at the Birth to Three Clinic at the University of Minnesota. She received a doctorate in educational psychology from the University of Minnesota and is a doctoral candidate in counseling psychology at the University of St. Thomas in Minneapolis, Minnesota. Her clinical and research work focuses on the intersection of trauma and neurodevelopmental disabilities with a focus on refugee populations.
Becky Carr, MA, is a doctoral candidate in clinical psychology at Augsburg University in Minneapolis, Minnesota. Currently, she is an advanced practicum student at the Birth to Three Clinic at the University of Minnesota where she is focused on providing early childhood mental health assessments. She has clinical experience in neuropsychological assessment and providing psychotherapeutic services to youth and families. Ms. Carr is also trained in the Circle of Security Parenting.
Matthew Mahoney, DO, is a pediatric resident physician at the University of Minnesota. He spends his time caring for children and their families at the University of Minnesota Masonic Children’s Hospital, Children’s Minnesota Hospitals, and Hennepin County Medical Center. His specific interests include improving how doctors communicate unexpected news, better understanding the impact of long-term hospitalizations on childrens’ mental health, and pediatric dermatology.
Claire Dahl was the clinical research coordinator in the Birth to Three Clinic at the University of Minnesota and is a current clinical psychology graduate student at the University of Delaware. Ms. Dahl has coordinated work exploring prevalence and presentation of neurodevelopmental and IECMH disorders in young children, with a focus on young children who have experienced trauma and chronic stress. She is interested in how chronic or intensive stressors affect young children, their caregivers, and the parent–child relationship as well as the bidirectional relationship between a child and their social environment and how related factors can be leveraged for intervention.
Nora Erickson, PhD, is a clinical child psychologist and assistant professor in the Department of Pediatrics, Division of Clinical Behavioral Neuroscience at the University of Minnesota Medical School. She received her doctorate in clinical psychology from Washington State University and completed a predoctoral internship and postdoctoral fellowship at the University of Michigan. Dr. Erickson’s clinical and research work focuses on the intersection between perinatal well-being and early childhood mental health, with a specific emphasis on trauma, toxic stress, and resiliency. Dr. Erickson has prior training in several evidence-based early childhood interventions, including intergenerational and group-based modalities.
Maria Kroupina, PhD, LP, is a clinical child psychologist and an associate professor in the Department of Pediatrics at the University of Minnesota Medical School and the Director of the Birth to Three and Early Childhood Mental Health Program. The overarching goal of Dr. Kroupina’s work is to understand and support vulnerable children by providing early assessment and intervention to support a positive trajectory for their future by both understanding and dismantling the impact of toxic stress on their development.
Suggested Citation
Parker-McGowan, Q., Carr, B., Mahoney, M., Dahl, C., Erickson, N., & Kroupina, M. (2023). University of Minnesota’s Birth to Three Clinic: comprehensive assessment and diagnosis across diverse settings ZERO TO THREE Journal, 43(4), 13-20.
References
Achenbach, T. M. (1999). The Child Behavior Checklist and related instruments. In M. E. Maruish (Ed.), The use of psychological testing for treatment planning and outcomes assessment (pp. 429–466). Lawrence Erlbaum Associates Publishers.
American Academy of Pediatrics. (2022). US child health care trends [PowerPoint slides]. https://downloads.aap.org/AAP/PDF/CHT_Child%20Health%20Care_Dec%202022.pdf
Dahl, C. M., Bauer, M. J., & Kroupina, M. (2023). DC:0–5 system in clinical assessment with specialty pediatric populations. Journal of Infant Mental Health (advanced online publication). https://doi.org/10.1002/imhj.22034. https://onlinelibrary.wiley.com/doi/10.1002/imhj.22034
Fallucco, E. M., Wysocki, T., James, L., Kozikowski, C., Williams, A., & Gleason, M. M. (2017). The brief early childhood screening assessment: Prelminary validity in pediatric primary care. Journal of Developmental and Behavioral Pediatrics, 38(2), 89–98.
Fisher, P. A., Leve, L. D., Delker, B., Roos, L. E., & Cooper, B. (2016) A developmental psychopathology perspective on foster care research. In D. Cicchetti (Ed.), Developmental Psychopathology (3rd ed., pp. 513–548). Wiley
Hartinger-Saunders, R. M., Jones, A. S., & Rittner, B. (2019). Improving access to trauma-informed adoption services: Applying a developmental trauma framework. Journal of Child & Adolescent Trauma, 12(1), 119–130. doi:10.1007/s40653-016-0104-1. https://link.springer.com/article/10.1007/s40653-016-0104-1
Leslie, L. K., Gordon, J. N., Ganger, W., & Gist, K. (2002). Developmental delay in young children in child welfare by initial placement type. Infant Mental Health Journal, 23, 496–516. https://doi.org/10.1002/imhj.10030. https://onlinelibrary.wiley.com/doi/10.1002/imhj.10030
Lieberman, A. F. (2004). Traumatic stress and quality of attachment: Reality and internalization in disorders of infant mental health. Infant Mental Health Journal, 25(4), 336–351. doi:10.1002/ imhj.20009. https://onlinelibrary.wiley.com/doi/abs/10.1002/imhj.20009
Mandalenakis, Z., Giang, K. W., Eriksson, P., Liden, H., Synnergren, M., Wåhlander, H., Fedchenko, M., Rosengren, A., & Dellborg, M. (2020). Survival in children with congenital heart disease: Have we reached a peak at 97%?. Journal of the American Heart Association, 9(22), e017704. https://doi.org/10.1161/JAHA.120.017704. www.ahajournals.org/doi/10.1161/JAHA.120.017704
Massie, H. N., & Campbell, B. K. (1983). The Massie-Campbell scale of motherinfant attachment indicators during stress. In J. Call, E. Galenson, & R. Tysons (Eds), Frontiers of Infant Psychiatry (pp. 394–412). Basic Books.
Mullen, E. M. (1995). Mullen Scales of Early Learning. National Academy Press.
Osofsky, J. D., & Lieberman, A. F. (2011). A call for integrating a mental health perspective into systems of care for abused and neglected infants and young children. American Psychologist, 66(2), 120–128. doi:10.1037/a0021630. https://psycnet.apa.org/doiLanding?doi=10.1037%2Fa0021630
Palmer, A. R., Dahl, C., Eckerle, J. K., Spender, M., Gustafson, K., & Kroupina, M. (2021). Early childhood mental health evaluation protocol within a multidisciplinary pediatric clinic for adopted and foster care children. Perspectives in Infant Mental Health. https://perspectives.waimh.org/wp-content/uploads/sites/9/2021/10/2021_2_Perspectives_IMH_29_10_2021_published.pdf
Pears, K., & Fisher, P. A. (2005). Developmental, cognitive, and neuropsychological functioning in preschool-aged foster children: Associations with prior maltreatment and placement history. Journal of Developmental & Behavioral Pediatrics, 26(2), 112–122.
Platt, C., & Gephart, S. M. (2022). Placement disruption of children with disabilities in foster care. Journal of Pediatric Nursing, 66, 30–35. https://doi.org/10.1016./j.pedn.2022.05.004. https://www.sciencedirect.com/science/article/abs/pii/S0882596322001178
Sachser, C., Berliner, L., Holt, T., Jensen, T. K., Jungbluth, N., Risch, E., Rosner, R., & Goldbeck, L. (2017). International development and psychometric properties of the child and adolescent trauma screen (CATS). Journal of Affective Disorder, 210, 189–195. https://doi.org/10.1016/j.jad.2016.12.040. https://www.sciencedirect.com/science/article/abs/pii/S0165032716313581?via%3Dihub
Sheldrick, R. C., Henson, B. S., Neger, E. N., Merchant, S., Murphy, J. M., & Perrin, E. C. (2013). The baby pediatric symptom checklist: Development and initial validation of a new social/emotional screening instrument for very young children. Academic Pediatrics, 13(1), 72–80. https://doi.org/10.1016/j.acap.2012.08.003. www.academicpedsjnl.net/article/S1876-2859(12)00202-1/fulltext
Shonkoff, J. P., Garner, A. S., Committee on Psychosocial Aspects of Child and Family Health, Committee on Early Childhood Adoption and Dependent Care, and Section on Developmental and Behavioral Pediatrics. (2012). The lifelong effects of early childhood adversity and toxic stress. Pediatrics, 129(1), e232–e246. https://doi.org/10.1542/peds.2011-2663. https://publications.aap.org/pediatrics/article/129/1/e232/31628/The-Lifelong-Effects-of-Early-Childhood-Adversity
Sparrow, S. S., & Cicchetti, D. V. (1989). The Vineland Adaptive Behavior Scales. In C. S. Newmark (Ed.), Major psychological assessment instruments, Vol. 2, pp. 199–231. Allyn & Bacon.
Zeanah, C. H., Boris, N. W., Heller, S. S., Hinshaw-Fuselier, S., Larrieu, J. A., Lewis, M., Palomino, R., Rovaris, M., & Valliere, J. (1997). Relationship assessment in infant mental health. Infant Mental Health Journal, 18(2), 182–197. https://onlinelibrary.wiley.com/doi/10.1002/(SICI)1097-0355(199722)18:2%3C182::AID-IMHJ7%3E3.0.CO;2-R
ZERO TO THREE. (2021). DC:0–5: Diagnostic classification of mental health and developmental disorders of infancy and early childhood, Version 2.0.

