Jennifer L. Harman, Memphis, Tennessee

Abstract
The opioid epidemic and related substance abuse reaches far and wide, with many newborns across the country left to endure the consequences. What follows is a unique, first-person account of a “Story From the Field” that highlights the experiences of one mother as she watched her adopted daughter suffer the effects of neonatal abstinence syndrome and as she repeatedly observed the absence of infant mental health supports within the context of her daughter’s treatment. This story elucidates the need for improved infant and early childhood mental health services within the context of treatment for neonatal abstinence syndrome.
“How you are is as important as what you do” is one of my favorite infant mental health quotes (Pawl & St. John, 1995). I have used it to anchor me as a professional for years—to help me remember to stay focused on the present and fully engaged. Yet, when meeting my daughter for the first time, and in each of the days since then, these words have rung true in a different sense.
Let me start by explaining a bit about my professional background. I am a pediatric psychologist with expertise in infant and early childhood mental health. Because of this background, I, like many readers, know that babies have feelings and that infancy and early childhood is the foundation upon which all other development is built. I understand how important it is for a caregiver to bond with their newborn, various factors that impact that bonding, and interactions and variables that promote bonding and a secure attachment. I know that relationships matter—starting from the very beginning, and that it is important to wonder about the internal state of your baby and to think about possible ways in which outwardly observable behaviors are linked to internal states. I also fully appreciate that a caregiver’s internal state can profoundly impact their baby and that babies rely upon their caregivers for co-regulation. What I did not know until becoming the mother of a baby with neonatal abstinence syndrome (NAS) was how hard I would need to fight for the care of my daughter to be consistent with infant and early childhood mental health principles and how much work the field has left to do in service to babies born with NAS.
Because of this, I feel compelled to tell our story. In doing so, I hope to raise awareness and interest in improving systems and supports provided to families of babies diagnosed with NAS. What follows is a brief, somewhat censored synopsis of events that includes information on our journey and what I believe the field can learn from our experience.
The Journey
I got the call that my daughter, Grace, was about to be born on a Tuesday morning—6 weeks and a day sooner than expected. I quickly loaded the car with baby essentials, toiletries, and a couple of outfits for myself. I drove through snow, sleet, rain, a lot of traffic, and 4 states. About an hour into my drive I got a picture and text message from one of the adoption case workers saying, “She’s here and she’s perfect!”
I finally arrived at the hospital where Grace was born. She was 12 hours old. I immediately felt my heart bursting with pride—she was, indeed, perfect and already loved beyond measure! Yet, by the time I left the hospital that night, I felt an enormous amount of worry. I was allowed to spend only approximately 2 hours with Grace that first night, because the adoption paperwork was not yet signed by her birth parents. However, over the course of those 2 hours I watched my daughter become spastic and jittery; and, I heard the sound of her cries begin to change.
When I returned to the hospital the following morning it became exceedingly evident that something was wrong. Grace’s cry was very high-pitched, shrill, and constant. She had frequent tremors, jerks, and twitches; and the skin on her bottom looked like it was eroding. Nurses came in every 2 hours, at minimum, and reported very high scores on the Finnegan Neonatal Abstinence Scoring System, a tool used to assess drug withdrawal in babies—higher scores indicate more symptoms and increased severity of symptoms (Finnegan & Kaltenbach, 1992).
Adjusting to a New Reality
Although I knew Grace’s birth mother had a prior substance abuse history, my understanding was that she had not used or abused any substances in well over 2 years. This was the information she provided to the adoption agency; and, thus, it was the information provided to me. I was not mentally prepared for the shock of what I was experiencing—or, quite frankly, the trauma of watching my tiny, sweet Grace, who I already loved so much, suffer so tremendously. I had not prepared for the adoption of a child with special health care needs, but that was the reality I faced. I was scared, and quite frankly a bit angry—not angry that Grace had special health care needs, but rather that she was suffering. The second I laid eyes on Grace I felt certain that she was meant to be my daughter and I was meant to be her mother. I never wavered in this belief. Perhaps because of this, I also felt guilt—guilt that I had not been able to somehow protect Grace from the torture she was experiencing, guilt that I did not somehow intuitively know what she was experiencing in utero, and guilt that I had not been able to do something to prevent her prenatal exposure to substances. Luckily, I recognized this guilt as misplaced and unwarranted. I also knew that getting lost in feelings of guilt, anger, and anxiety was of no benefit. I knew that my baby needed me to be able to think clearly, to stay regulated, and to remain present-focused, attentive, and responsive. I knew Grace needed and deserved to experience the best of me and as much nurturance as possible—I knew all of this because of my professional training and background.
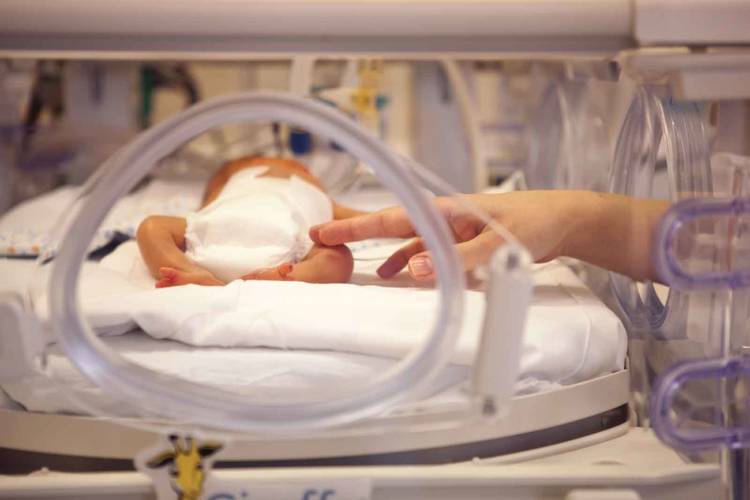
Treatment of babies with neonatal abstinence syndrome should include support services targeted at helping parents remain emotionally regulated. Photo: Pushba/shutterstock
Because of this, I implemented mindfulness, positive self-talk, diaphragmatic breathing, and reframing strategies like I never have before. These strategies helped me mentally shift and adjust to our new reality.
Grace required continuous treatment under bili blankets and bili lights, a type of light therapy to treat jaundice, for 7 days. Because of these treatments I was initially permitted to hold her for only a few moments a day. Throughout her first month Grace also periodically required supplemental oxygen; and she had to have her blood drawn every 2 hours due to difficulties with blood glucose stabilization. She had frequent runny stools and lost 14% of her initial birth weight in a matter of days. I was eventually told this rapid weight loss was due not only to her obvious inability to coordinate her sucking, swallowing, and breathing, but also due to the high amount of energy expended on a constant basis as a result of her withdrawal. This weight loss coupled with her feeding difficulties necessitated placement of a nasogastric feeding tube for supplemental nutrition. She sneezed many times a day, consistently slept for less than an hour between feeds, and often took shallow, rapid breaths.
On Grace’s fourth day of life her birth parents signed the necessary paperwork and I was able to legally take on my role as primary caregiver. At this point, I inquired about holding Grace during feedings or briefly after diaper changes, noting that I understood it was still imperative that she remain under the bili lights as much as possible. At first the nurse seemed leery of my question; she even commented “Oh! Grace won’t remember these early days. There will be time to hold her.” However, she obtained permission from the neonatologist and I was finally able to hold my baby for more than a few moments at a time. Interestingly, Grace’s tachypnea, or rapid, shallow breathing, improved when being held, particularly when being held skin-to-skin.
Grace was eventually moved to a neonatal intensive care step-down unit, which allowed me to room in with her. During my caregiver orientation for the step-down unit I was instructed that I was not allowed to leave the room unless another caregiver was present and the nurse assigned to Grace for that shift knew where I was going and when I would return. I was shown how to contact the nurse for a general need and how to contact the nurse for emergencies; but, I was also reassured that Grace would remain hooked up to monitors that would alarm at the nurses’ station when (not if) her oxygen levels dropped below acceptable levels. I was then provided with a long list of additional things for which to watch that could constitute an emergency. It was very scary, but I was thankful they were honest with me; and I was thankful they were finally able to openly share information regarding Grace’s condition with me. I also found myself incredibly thankful for previous experiences working with and around very medically fragile babies. Without that previous lived professional experience, I do not know how I would have felt when faced with the daunting task of managing such complex needs. Had I been not used to being around very fragile babies or if I didn’t “speak medicalese,” the adjustment would have been even more difficult.
The room was small and dark—though this was not necessarily a bad thing for Grace, and I was of the mindset that anything that was good for Grace was good for me. The neonatology fellow and I both observed Grace’s tremors and cries significantly worsening whenever the room was illuminated. As such, I was more than happy to oblige when encouraged to keep the lights low or off and to avoid turning on the television. I was willing to do anything that might potentially help my girl! I remained in that room, loving my daughter through the most unbearably difficult situation for weeks. Indeed, the infant mental health savvy neonatology fellow often told me the best thing anybody is able to do for a baby experiencing the devastating effects of withdrawal is to love them through it.
After about a month we were discharged from the hospital— Grace had learned to take a bottle, and when fed small amounts every 90 minutes could tolerate feeds by mouth. She was slowly weaned off all medications (e.g., morphine) given to her to help lessen the severity of her withdrawal symptoms and in efforts to avoid withdrawal-related seizures. She continued to have tremors, myoclonic jerks, and some hypertonia; however, these symptoms certainly were improved from those first few weeks. She also continued to have a shrill cry and periods of time where she was exceedingly difficult to soothe—but Grace had come so far in a month’s time. She clearly and repeatedly demonstrated her strength and resilience very early in life. I knew she would be okay; I knew we would be okay. My baby is strong and has proven she can overcome just about anything!
The Necessity of Self-Care
Being a psychologist who specializes in infant and early childhood mental health, I knew several things that were needed to promote Grace’s overall well-being. First, I needed to be able to take care of myself and my mental health, as Grace’s functioning was heavily dependent upon my own. Words do not exist to describe how difficult it is to watch your baby suffer all day, every day. Thankfully, my mother came to assist me after I spent the first week in the hospital with Grace. Her presence allowed me to take short, 15–20 minute breaks once a day where I walked around the hospital or surrounding neighborhood. Those brief breaks allowed me time to clear my mind and were paramount to preserving my mental health. On those walks, and many times since this experience, I wondered how a parent who does not have someone willing and able to come assist manages in those early weeks and months of loving a baby through withdrawal. With this in mind, I urge those who work in hospitals and other settings that provide care for newborns with NAS to consider ways to support opportunities for caregivers to tend to their own well-being—if only for 15 minutes a day when isolated in the hospital setting.
Relatedly, I also knew that it was of utmost importance for me to remain emotionally regulated for a number of reasons, including to help Grace co-regulate. Because of this I practiced mindfulness, breathing exercises, and positive self-talk daily. In the plethora of caregiver trainings provided to me at the hospital where Grace was born, nobody ever mentioned the importance of remaining regulated and calm or strategies to facilitate this. Luckily for me, and for Grace, doing so is well within my professional wheelhouse and remained at the forefront of my mind. Meanwhile, I found myself pondering whether caregivers without training similar to mine would intuitively know this. I am sure some would, but others may not.
Infant and Early Childhood Mental Health and NAS
The infusion of infant and early childhood mental health principles into the treatment of babies with NAS is essential. Specifically, treatment of babies with NAS should include support services targeted at helping parents remain emotionally regulated. Parents could be taught mindfulness, acceptance-based cognitive strategies, and relaxation strategies such as diaphragmatic breathing and progressive muscle relaxation to help them remain regulated. Parents would undoubtedly also benefit from supportive active listening and guidance regarding use of parental reflective functioning, or consideration of the internal state of their baby. Medical staff should remain cognizant that, although they may see suffering like this somewhat regularly, most parents do not. As such, they should try to remain sensitive to how the experience is affecting parents. In fact, watching human suffering is hard on anybody— including those who see it day in and day out. As such, medical staff would likely benefit from opportunities to engage in reflective supervision and consultation. The sensitivity and responsivity of medical staff would likely increase if they are given opportunities to step back from their immediate, intense professional experiences to consider their own thoughts and feelings about the care environment and the potential impact of their thoughts and feelings on the care of the baby and family.
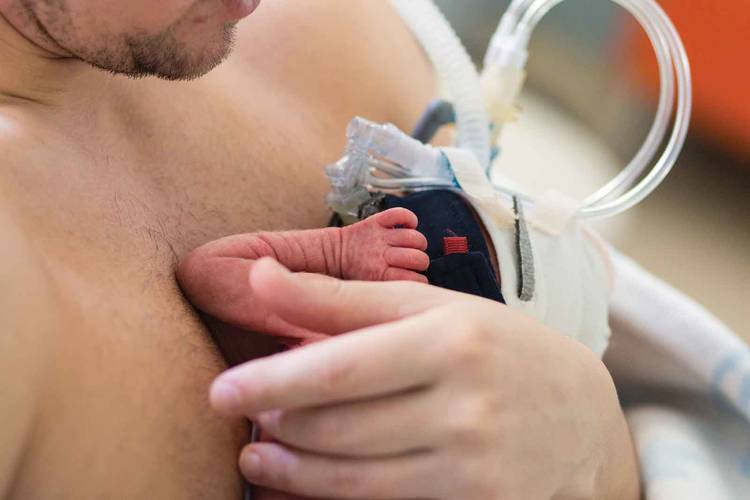
Education regarding the importance of touch for both the parent and the baby should be provided to parents and all medical staff alike; and protocols for ensuring safe skin-to skin contact should be implemented, encouraged, and celebrated whenever possible. Photo: Katrina Besselova/shutterstock
Parents’ perceptions of the difficulties they experience watching the intense suffering of their baby should be validated and considered when explaining to them any additional responsibilities the medical team would like for the parents to take (e.g., how to identify a medical emergency and contact a nurse). Direct education should be provided to parents of babies with NAS regarding the importance of taking care of their own mental health so they are able to provide the type of calm, attentive, responsive care their baby needs. Finally, education regarding the importance of touch for both the parent and the baby should be provided to parents and all medical staff alike; and protocols for ensuring safe skin-to skin contact should be implemented, encouraged, and celebrated whenever possible.
Where We Are
The first 4 months of Grace’s life were consistently torturous for her and absolutely heartbreaking for me. The fifth and sixth months of her life were colored by the periodic reemergence of withdrawal symptoms; yet, these symptoms were much less severe than during the first 4 months. She was extremely well loved through every second of misery she experienced; and I was well supported through it all. I called on all of my resources to stay grounded and calm; and I put into practice every skill I have ever clinically assisted a parent of an infant garner. I am fortunate that I was able to call upon that training to guide me as I entered parenthood amidst what felt like a crisis. I believe with certainty that those skills, mentioned above, and the supports provided to us through our state’s early intervention system, including physical therapy and familycentered, routines-based developmental therapy services, are why Grace is now described as “thriving,” “catching up,” and “largely on-target developmentally.” I also believe it is why she laughs and smiles and exudes such glee on a daily basis. She is one of the strongest human beings I know; she is resilient and amazing—she is my hero.
Learn More
Additional information related to neonatal abstinence syndrome: www.cdc.gov/pregnancy/features/public-health-reporting-of- NAS.html
www.aamc.org/news-insights/caring-babies-opioidwithdrawal
Neonatal Abstinence Syndrome R. N. McQueen & J. Murphy-Oikonen (2016) New England Journal of Medicine, 375, 2468–2479
Neonatal Abstinence Syndrome P. Kocherlakota (2014) Pediatrics, 134(4), e547–e561
Author Bio
Jennifer L. Harman, PhD, is a pediatric psychologist, assistant faculty member, and assistant director of the Psychology Clinic at St. Jude Children’s Research Hospital. She received her doctorate from the University of Florida and specializes in work with very young children and their families.
Suggested Citation
Harman, J. L. (2020). Perspectives: Loving my baby through withdrawal: Infusing principles of infant and early childhood mental health in the treatment of neonatal abstinence syndrome. ZERO TO THREE Journal, 40(6), 50–53.
References
Finnegan, L. P., & Kaltenbach, K. (1992). Finnegan Neonatal Abstinence Scoring–Neonatal abstinence syndrome. In R. A. Hoekelman, S. B. Friedman, N. M. Nelson, & H. M. Seidel (Eds.), Primary pediatric care (2nd ed.). St. Louis, MO: Mosby.
Pawl, J., & St. John, M. (1995). How you are is as important as what you do…in making a positive difference for infants, toddlers, and their families. Washington DC: ZERO TO THREE.




