Pamela Scorza and Catherine Monk, Columbia University Medical Center, New York, New York

Abstract
The transition to parenting (Galinsky, 1987) can be a tumultuous time, particularly when parents have experienced traumatic and stressful life circumstances. Interventions to help these parents often focus on the first 2 years after birth because of the importance of this sensitive period for babies’ developing brains. However, we describe research showing that babies’ experiences in the womb matter just as much as the experience after birth. We give examples of interventions to support expecting parents by addressing prenatal stress and trauma. These types of intervention can help in the transition to parenting and promote positive development for both parents and their future children.
Yasmina can’t shake the horrible feeling that something will go wrong before her baby is born. Her immigration status is a constant threat, and she hesitates to use medical services unless she absolutely has to. Her landlord is threatening to kick her and her boyfriend out because they’re late paying rent. Her boyfriend often comes home drunk, if he comes home at all, and Yasmina is afraid he is going to leave her because of the responsibility that the new baby will bring. Sometimes she wonders if she actually wishes something would go wrong before the baby is born. That thought makes her feel guilty and worse about herself than she normally does. Why does she always get herself into terrible situations like this? What kind of mother is she going to make, and what kind of life is she going to be able to provide for this baby?
Luckily, a friend told Yasmina about a clinic for prenatal care where the staff wouldn’t ask about her immigration status. The clinic even had behavioral health services for mental health problems integrated into the prenatal care visits. Through a process of supportive counseling, Yasmina and her therapist identified some “ghosts in the nursery” (Fraiberg, 1995). Yasmina’s father was killed when she was very young, and she was exposed to a great deal of violence when she was growing up. Her mother was overwhelmed trying to take care of her and her sisters, and she often left them alone in their dangerous neighborhood for several days while she went to the city to try to earn some money for the family. Later, when Yasmina made the arduous journey to the United States, she was raped.
Her therapist made Yasmina feel like someone really cared about her and was equipped to help her overcome her fears. The therapist helped Yasmina see how her boyfriend’s absences made her feel emotionally abandoned as she had felt as a child, and full of protest and criticism as she couldn’t do when she was younger. Unfortunately, her responses contributed to his pulling away more, which made her feel worse. In addition, the trauma from her past was held in her body; her shoulders tightened and her breathing became shallow every time she thought about her past or about her fears for the future. Yasmina learned mindfulness techniques that helped her gradually work through this stress in her body. Her therapist also made sure that a social worker helped Yasmina secure temporary housing when she was eventually kicked out of her apartment and connected her with other resources Yasmina needed. The therapy focused not only on Yasmina’s past and her vision for the future but also helped her start to connect with her baby, to envision the possibility that she could care for her baby as she wished she had been cared for when she was a child. Through the course of therapy, Yasmina started to realize how much she already cared about her baby and that she had tools and support to start a new kind of life for her and the baby.
Stress in pregnancy is a common experience for many parents, particularly for those who have a history of past trauma. Poverty, family instability, and traumatic events from childhood or more proximal periods can make the transition to parenthood a particularly rocky time. Interventions to help at-risk parents often focus on the period after birth when the baby is young because research has shown that parents’ stress and trauma can affect caregiving, and thus the baby, at this crucial postnatal time of brain development.
Yet a baby’s development actually begins long before birth. Independent of what happens after the baby is born, maternal stress (which often includes associated symptoms of anxiety and depression) can put babies at higher risk for poor development and mental and physical health problems throughout their lives. It is relatively recent that researchers have been able to probe beyond the woman’s pregnant belly to understand how prenatal stress can affect the baby’s in utero development. In this article we describe potential pathways by which prenatal stress can affect fetal development.
Parents who have experienced trauma in their own childhood or as young adults often find the transition to parenting especially stressful. Many women who are depressed or anxious in pregnancy have experienced early trauma, and evidence suggests that early trauma predicts prenatal depression even more so than it predicts postpartum depression (Blackmore et al., 2013). The ongoing effects of their own trauma can make it difficult for parents to manage the typical anxiety every woman experiences during pregnancy such that they have much higher levels of it. Pregnancy is a time when expecting parents may reflect on their own childhood experiences with their parents, and painful memories can become activated. Prenatal parenting for this group must address parents’ own trauma and work to build a bond with their future baby. We describe interventions during the transition to parenting that address stress and trauma during pregnancy and help expecting parents develop the confidence that they can give their child a brighter future than the past that they experienced.
Maternal Distress Gets Under Fetal Skin
Any woman who has been pregnant can relate to the excitement of imagining the baby’s development in the womb—the little fingers and fingernails growing, the tadpole-like tail giving way to little legs and tiny toes, the eyes that even start to blink in the womb. Just as the fetus’ organs and limbs are developing, its brain is growing billions of neurons and intricate circuits connecting them. Scientific evidence now shows that parents’ mood, lifestyle, and life circumstances can have a significant effect on the developing baby’s brain (Anderson & Thomason, 2013). In utero, fetuses of mothers with prenatal depression show greater reactivity to stress (measured by their heartbeat changes), and once they are born, they show alterations in the connections between brain regions (Posner et al., 2016). Because the foundations of the central nervous system develop prenatally, small changes during this critical period can impact subsequent neural network patterns and have significant relevance for neurobehavioral development.
Fetal programming is the concept that the environment in the womb can affect the development of a fetus and can have long-lasting impacts on the child (Barker, 1990). If a mother is stressed, anxious, or depressed while she is pregnant, the child is more likely to be born early and to be small for its age. Maternal distress during pregnancy also predicts behavioral problems in babies and children as they grow, including externalizing problems, anxiety and depression, and other kinds of psychiatric disturbances (van den Bergh et al., 2017). These children also are more likely to have health problems and more trouble learning and developing healthy relationships.
How Does Maternal Distress Get Under the Fetal Skin?
After the baby is born, it is simpler to study the relationship between a parent and the infant. Researchers can observe behavioral interactions between the parent and infant, measure the mother and baby’s vital signs, and even take blood samples to examine molecular and genetic factors. But researchers have also taken on the challenge of understanding the complex interactions between parents and their children while the baby is still in the womb.
In our work, we directly “ask the fetus questions” in relation to maternal distress levels, and we also examine newborn brain development and infant behavior. For example, we and others (DiPietro, Costigan, Hilton, & Pressman, 1999; DiPietro, Hodgson, Costigan, & Hilton, 1996; Monk et al., 2010; Monk et al., 2000; Monk et al., 2004; Pressman, DiPietro, Costigan, Shupe, & Johnson, 1998; Sandman et al., 1994) have found that fetuses are more reactive to stimuli and vary in other ways in their neurobehavorial development when their mothers are anxious or stressed. To test for these differences, fetal heart rate and movement are collected via Doppler-based transducers while women undergo different laboratory experiences. Newborns sleep during MRI-based brain imaging sessions, and infants as well as toddlers are assessed in established protocols to study temperament, fear responses, and cognitive abilities (Cao, Laplante, Brunet, Ciampi, & King, 2014; Gustafsson et al., 2018; Laplante, Brunet, & King, 2016; Werner et al., 2007).
Research on fetal programming has revealed several pathways by which parents’ prenatal stress can get under the fetal skin, that is, affect fetal brain and future neurobehavioral development.
Hypothalamic-Pituitary-Adrenal Axis and the Placenta
The hypothalamic-pituitary-adrenal (HPA) axis is a central component of the stress response system. It is responsible for secreting the stress hormone cortisol, which alerts the organism to potential threat and maintains homeostasis. Prenatal maternal distress is associated with dysregulation of the maternal HPA axis, which can lead to higher levels of circulating stress-associated hormones (Thayer, Wilson, Kim, & Jaeggi, 2018).
These hormones can affect placenta functioning and cross the placenta, reaching the fetus (Monk et al., 2016). Although the placenta may seem very expendable, and is usually discarded after birth, it plays a crucial role in the fetus’s development by regulating the chemicals and hormones that pass from the mother to the baby during pregnancy. Maternal stress, depression, or trauma can change the way the placental functions, making it less able to protect the developing baby from the stress chemicals that could impact its development (Brunst et al., 2017; Glombik et al., 2015; Lambertini, Chen, & Nomura, 2015). Research shows that this change in placental function can be one way by which maternal distress affects the development of the offspring’s HPA circuitry as well as brain circuitry, thereby increasing the risk for psychopathology later in life.
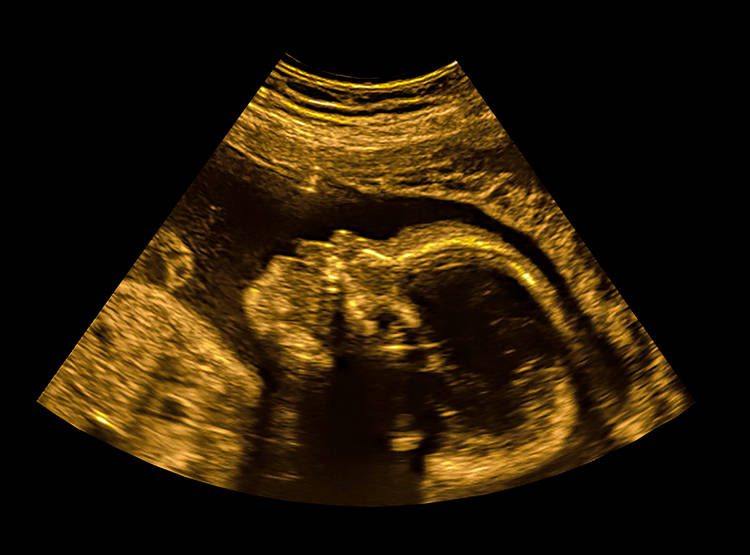
Just as the fetus’ organs and limbs are developing, its brain is growing billions of neurons and intricate circuits connecting them.
Gut Microbiome
It’s not only the placenta that can communicate mothers’ distress to the developing fetus. The bacteria in human intestines plays an important role in health and disease, including neurodevelopment and psychiatric functioning (Lima-Ojeda, Rupprecht, & Baghai, 2017). Studies have shown that people with depression, stress, and anxiety have different bacteria living in their intestines (Cenit, Sanz, & Codoner-Franch, 2017). Prenatal stress is known to alter maternal microbiota composition, and this suboptimal gut flora might get passed along to the infant, either during birth, or earlier through the placenta or amniotic fluid (Culhane et al., 2001), altering the baby’s developing brain.
Sleep, Obesity, Nutrition, Other Diseases—and Dads
During pregnancy, sleep can be affected by reproductive hormones and physical discomfort from pregnancy. Pregnant women might sleep more during the first trimester because of constant fatigue, but it is often difficult to get a good night’s sleep in the third trimester. Stress, depression, and trauma can make sleep even more elusive. When a pregnant woman doesn’t sleep well during pregnancy, stress hormones can increase, and again, these elevated hormone levels can pass through the placenta to the fetus, interfering with brain development.
Expecting women who are experiencing stress and trauma often also aren’t eating a healthy diet, which is another way parental stress can affect the baby before birth. Researchers first discovered that prenatal diet affected child outcomes when they studied children whose mothers were pregnant during the Dutch famine of 1944–45. During this Hongerwinter, a German blockade cut off food shipments from farm towns located in the western provinces north of the great rivers. At least 22,000 died and many more were kept alive thanks to soup kitchens. Children conceived during the Hongerwinter had higher risk of disease later in life, including mental disorders. Through additional studies, researchers have found that when pregnant women don’t get enough food in general, or they don’t get enough of specific micronutrients, such as zinc and iron, or vitamins, such as folate and vitamin A, their children are more likely to develop cognitive delays, attention deficit/hyperactivity disorder, and psychiatric disorders.
Having too much food also can be a problem. When parents are experiencing stress or trauma, they may try to cope with their emotions by reaching for “comfort foods.” Those cookies and chips and other high fat, sugary, processed foods affect women’s biology, which can also lead to the development of depression (Sánchez-Villegas et al., 2012; Sánchez-Villegas et al., 2011; Vermeulen et al., 2017). When an expecting mother, or even father, has obesity, the baby is more likely to be born unhealthy or suffer more health problems as it develops.
Psychological distress is also related to infection (Cohen, Tyrrell, & Smith, 1991) as well as diseases such as diabetes (Hackett & Steptoe, 2017) and hypertensive disorders such as preeclampsia (Zhang et al., 2013), which even at the preclinical level could contribute to offspring’s risk for psychopathology. Pregnant women with chronic disease often are highly anxious, in particular in relation to their pregnancy outcomes. Several lines of evidence from human and preclinical models suggest that diabetes onset is influenced by psychological stress (Hackett & Steptoe, 2017). Also, a study showed that psychosocial stressors may be associated with gestational diabetes mellitus onset (Horsch et al., 2016). Pre-gestational diabetes and gestational diabetes mellitus have been associated with altered cognitive outcomes in the offspring (Adane, Mishra, & Tooth, 2016) and with increased risk for Autism Spectrum Disorder (Sacks et al., 2016; Xiang et al., 2015).
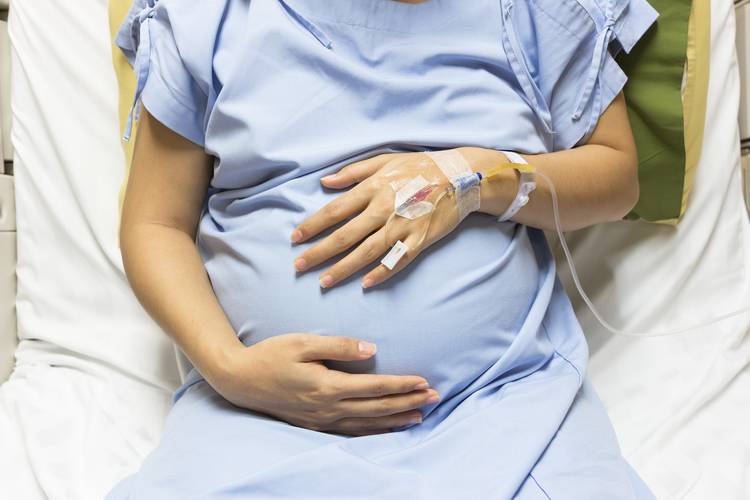
A mother’s psychological stress as well as infections and diseases could impact the fetus through the mother’s immune response to these conditions.
A mother’s psychological stress as well as infections and diseases could impact the fetus through the mother’s immune response to these conditions. Immune cells that pump out cytokines in response to invaders (or even stress) are involved in neuron growth and survival (Marx, Jarskog, Lauder, Lieberman, & Gilmore, 2001). New research has documented that a mother’s immune activation is related to decreased fetal heart rate variability (one way of seeing early indication of emotion regulation in the fetus), and to alterations in brain structure and connectivity between brain areas (Rudolph et al., 2018; Spann, Monk, Scheinost, & Peterson, 2018). Together, these studies suggest that prenatal exposure to immune activation can impact the early development of the autonomic nervous system and brain networks involved in cognition, sensory processing, learning, and emotion.
A father’s lifestyle might even impact the future child. Studies in animal models suggest that paternal obesity and certain chemical exposures could be transmitted to the unborn baby through his sperm. For example, it is well known that maternal smoking, alcohol use, and drug consumption during pregnancy can affect fetal development. However, evidence from animal studies suggests that paternal alcohol consumption may also have an effect on the offspring, reducing cognitive development, and increasing anxiety and depression, through changes in the expression of genes in the sperm (Liang et al., 2014).
Structural Inequities
Racial inequities and racism, poverty, and violence contribute to life stress, often acting as the root causes of prenatal stress and its effects on infants. Research indicates that blacks in the US on average show accelerated biological aging, measured by biomarkers like length of telomeres, the ends of chromosomes in genes. This “weathering” is thought to be caused by the accumulated stress of racism and living as a minority. It is also implicated in the widening gap between rates of maternal mortality in blacks compared to whites in the US (Forrester et al., 2018).
Structural interventions ultimately need to address inequalities in housing, nutrition, air quality, health care, education, and the criminal justice system. While these inequities are being addressed, though, prenatal parenting interventions can help expecting parents cope in healthy ways with the stress or trauma in their lives. Often it is hard to change quickly factors in peoples’ lives, yet it is possible to change how they hold the experiences in their minds, the meaning made of them, the feelings associated with them, and tools used to cope.
Prenatal Parenting
These complex and largely hidden processes that connect mothers and their future children mean that supporting women who have experienced trauma or are highly stressed, or both, can start before birth—for their benefit as well as that of their future children. Prenatal interventions can help expecting parents cope in healthy ways with the stress or trauma in their lives so that the biological effectors of their stress are diminished and do not affect their future child (see Box 1). This intervention could include stress reduction techniques such as mindfulness as well as strategies to build healthy diets and exercise, even in the face of challenging emotions and traumatic situations.
Box 1. The Importance of Prevention
For the first time ever, the U. S. Preventive Services Task Force recently recommended focused depression interventions (1) for pregnant and postpartum women (versus the overall adult population) with the awareness that helping women also helps their children, and (2) that aim to prevent depression before it emerges (O’Connor, Senger, Henninger, Coppola, & Gaynes, 2019). This is precisely the shift that is needed in public health policy: an approach to mental health issues that includes the continuum of distress, aims to reduce stigma, and emphasizes providing help before disorders emerge. The authors are very pleased that our intervention, Practical Resources for Effective Postpartum Parenting, was included in the data leading to this new and important recommendation.
In addition, one key way to support expecting parents in their transition to parenthood (Galinsky, 1987) is to help them with a somewhat more apparent process, which is how they hold the child in their minds (and hearts) prior to birth. Addressing the biological stress transmission to the baby, as well as mothers’ mental states, are two, interrelated foci of prenatal interventions.
When Leah, a 16-year old from the Bronx, was pregnant, she felt alone and anxious; her childhood had been one of isolation and sadness, except for a close connection she felt with a supportive aunt who lived nearby. When a sonogram technician told her that she was the only one who knows her baby’s heartbeat, her aunt was with her, and she felt a surge of warmth for her baby and future role as a mother, a new source of calming feelings in her life, and new psychological representations of herself as a mother and of her future baby. This is the sort of moment that can contribute to future change, especially when identified through supportive prenatal interventions. One such intervention is Carnegie Hall Musical Connections group (Carnegie Hall Lullaby Project, 2011) that regularly holds sessions at prenatal clinics in New York City. A mother similar to Leah created a tune and several verses to express the same kind of feeling Leah had. With a lilting melody and violin accompanying, the chorus of her lullaby begins “You’re the only one who knows my heartbeat. And I’m the only one who knows your heartbeat.” One verse notes, “Starting from a new beginning, I’m going to show you how to be strong, gentle and loving, knowing right from wrong, be courageous, stand tall. Feel the power of my love, even when we are apart.”
Before birth, fetuses register sensory experience, and there is even evidence of learning that occurs as a fetus identified in what the baby remembers after its birth (Busnel et al., 2017; Moon & Fifer, 2000) Later in pregnancy, babies can tell the difference between different musical tones and short melodies, and as newborns, they have a preference for their mother’s voice over other women’s voices (Busnel et al., 2017). The feelings of bonding or attachment from mother to baby, and baby to parent, start prenatally.
Just like the young expecting mom Leah experienced, listening to a baby’s heartbeat can be a profound experience that can help to catalyze the bonding process. Programs within prenatal care clinics can capitalize on this by integrating focused time for expecting parents to connect with their babies. Although this prenatal connection is most often considered between the pregnant woman and her future child, a partner also can start to have feelings of attachment prenatally. Getting a jump start on positive bonding could set parents on track to have a stronger relationship with their child after birth, which could help put the child on course to develop healthy cognitive and emotional skills.
When expecting parents are allowed to dwell in the experience of being connected to the new life inside the mother, they might also feel a therapeutic respite from the stress and trauma in their own lives. In a new life, there is new opportunity.
Dad’s role is just as important as mom’s in prenatal parenting. If the father is an active participant in the mother’s life, his actions can affect her emotional state, and he can support or alternatively upset her. An abusive partner can be detrimental to a woman’s prenatal emotional state, whereas a supportive partner may buffer her against depression or anxiety.

Prenatal interventions can help expecting parents cope in healthy ways with the stress or trauma in their lives so that the biological effectors of their stress are diminished and do not affect their future child.
Prenatal Interventions That Can Make a Difference
All this research suggests that interventions with the parents to improve child outcomes should start before birth, such as the examples that follow.
Nurse-Family Partnership
Relatively few interventions start during pregnancy and follow the outcome for the child, but those that do show promise. The most studied is the Nurse-Family Partnership (Olds, Kitzman et al., 2004; Olds, Robinson et al., 2004), a home-visiting program targeted at lower income mothers, sometimes specifically teenage ones. This manualized program starts in pregnancy with visits from specially trained nurses and continues for the next 2 years. The nurses act as an overall support person for the mothers, but they also teach aspects of parenting and help with advice about nutrition and other aspects of a healthy lifestyle. The children have been followed up into early adulthood and show improvement, with particularly women being less likely to be involved in the criminal justice system and less likely to be on government benefits (Eckenrode et al., 2010).
Practical Resources for Effective Postpartum Parenting (PREPP)
Most expecting women who experience stress and trauma don’t get the help they need during pregnancy because of the stigma associated with mental health care and because of logistical barriers to attending added health care appointments. Programs that do exist are rarely situated within obstetrical care, and they usually don’t take advantage of the unique mother–infant dyadic orientation of the childbearing period.
PREPP is a new program that stands out as an exception. PREPP enrolls distressed pregnant women during the third trimester and continues through the 6-week postpartum check up. It includes four in-person “coaching” sessions that take place when the woman goes to her obstetrical, prenatal, and postnatal appointments. It also includes one check-in session by phone 2 weeks after the baby is born.
PREPP helps women develop mindfulness skills and parenting skills, and it helps them understand more about their own stress and trauma. To give the women practical tools to help ease the pressure during parenting, five specific infant behavioral techniques are taught. Each of these techniques is supported by emerging research and aims to reduce infant fussing and crying behavior and promote sleep (Barr et al., 2009; Meyer & Erler, 2011; Pinilla & Birch, 1993; St James-Roberts, Sleep, Morris, Owen, & Gillham, 2001; van Sleuwen et al., 2007). PREPP views prenatal depression as a potential disorder of the dyad, and it uses mother–infant behavioral interactions, infant regulation, and parenting competence, which are central components in improving maternal mood. The intervention aims to treat at-risk women by promoting maternally mediated behavioral changes in their infants.
As part of the intervention, women also were provided with counseling that encourages them to reflect on their own childhood and how it will impact the way they see themselves as mothers. They also learn mindfulness techniques to help them cope better when their babies are distressed or unable to be soothed and to help them to return to sleep after tending to their babies during the nighttime. Learning these skills before the baby is born helps women feel the confidence that they have tools to deal with the difficult aspects of having a newborn.
Lullaby Project
In the preceding vignette, we described Leah’s experience with the sonogram and an example of a woman writing a lullaby for her future child. Some women are fortunate to be part of a program run through Carnegie Hall in New York called the Lullaby Project. This powerful initiative invites pregnant woman who experience adversity or trauma to work with experienced, professional musicians to write lullabies for their babies. The lullabies are professionally recorded and performed live in Carnegie Hall. The Lullaby Project gives women an outlet for creativity, a way to confront and accept how they are feeling (Carnegie Hall Lullaby Project, 2011). It shows them their own strengths and allows them to imagine new possibilities. Some women continue writing poetry for their children. Others become more active in their community, organizing events or providing support to other young women in facing the same circumstances. Similar therapy interventions focus specifically on the power of narrative (Pennebaker, 2000) and self-reflection (Slade et al., 2005). The “light touch” Lullaby Project puts feelings into words, promoting self-regulation, self-reflection, and the possibility of agency in making the future different from the past.
MUMentum Pregnancy
The MUMentum Pregnancy program in Australia is a brief self-guided internet-based cognitive behavioral therapy intervention tailored specifically to women who experience anxiety and depression during pregnancy. The course introduces women to core cognitive behavioral therapy skills to help manage anxiety and depressive symptoms. The course is presented as an illustrated story, in which two characters experiencing anxiety and depression during their pregnancy learn to self-manage their symptoms. Each lesson follows the characters as they learn skills such as challenging their negative thoughts and learning to take small steps to build positive and healthy thought and behavior patterns. Each lesson includes an action plan as well as resources about sleep hygiene and other therapeutic practices. Initial studies suggest that Mumentum Pregnancy is well accepted and improves maternal mood, particularly anxiety and distress (Loughnan et al., 2019). Current efforts are underway to scale up the program.
Conclusion
Parents can affect the development of their child, even before birth. This might seem like both a blessing and a curse. For expecting parents who experience stress and trauma, and entrenched structural inequities, it might seem like the odds are stacked against them. The myriad pathways by which research suggests their life stress might influence their future child might make positive parenting seem doomed from the start based on the pull to repeat established relationship templates and maternal stress transmission to the baby before birth. Fraiberg and her colleagues introduced the metaphor “ghosts in the nursery” (Fraiberg, Adelson, & Shapiro, 2003) in 1975 to describe how parents unconsciously repeat the parenting patterns from their own childhood, as shown in the case of Yasmina at the beginning of the article.
More recently, though, Lieberman and her colleagues proposed that “angels in the nursery”—deep experiences of parent–child bonding where the child feels understood, accepted, and loved—have the power to break this cycle (Lieberman, Padron, Van Horn, & Harris, 2005). Prenatal parenting is a golden opportunity to place angels in the nursery and help women’s psychobiological well-being, for them, and the child to come. It is a time even more ripe for intervention than after birth because positive patterns can be set even before the exquisite complexity of a new baby has entered parents’ life. Programs to support expecting parents can capitalize on this moment by providing support and resources to make the transition to parenthood not only a new birth for the infant but a new beginning for the parents.
Learn More
Prenatal Developmental Origins of Future Psychopathology: Mechanisms and Pathways. C. Monk, C. Lugo-Candelas, & C. Trumpff (2019). Annual Review of Clinical Psychology, 15.
Development and parenting begin before birth. Epidemiological and observational clinical data demonstrate that maternal distress is associated with children’s increased risk for psychopathology: For example, high maternal anxiety is associated with a twofold increase in the risk of probable mental disorder in children. This article reviews several hypothesized biological systems by which maternal distress affects fetal and child brain and behavior development. It also discusses clinical implications of studies of the developmental origins of health and disease that focus on maternal distress.
Carnegie Hall Lullaby Project Hear a sample of one of the lullabies: Source link
About the Authors
Pamela Scorza, ScD, MPH, is a research fellow in the Department of Psychiatry at the Columbia University Medical Center. Her research examines biological and behavioral factors in the intergenerational transmission of mental health risk. With a background in global health and psychiatric epidemiology, she brings a population-based and prevention focus to translational research on interventions to interrupt cycles of adversity.
Catherine Monk, PhD, is a professor of medical psychology in the Departments of Obstetrics & Gynecology and Psychiatry and director of research at the Women’s Program at Columbia University Medical Center. Trained as a clinical psychologist, Dr. Monk’s research brings together the fields of perinatal psychiatry, developmental psychobiology, and neuroscience to focus on the earliest influences on children’s developmental trajectories. She is internationally recognized for her contributions to the Developmental Origins of Health and Disease Research model as they relate to prenatal exposure to maternal stress and depression. Her research is funded by the National Institutes of Health as well as by the March of Dimes, the Robin Hood Foundation, and Johnson & Johnson.
Suggested Citation
Scorza, P., & Monk, C. (2019). Anticipating the stork: Stress and trauma during pregnancy and the importance of prenatal parenting. ZERO TO THREE Journal, 39(5), 5–13.
References
Adane, A. A., Mishra, G. D., & Tooth, L. R. (2016). Diabetes in pregnancy and childhood cognitive development: A systematic review. Pediatrics, 137(5), e20154234.
Anderson, A. L., & Thomason, M. E. (2013). Functional plasticity before the cradle: A review of neural functional imaging in the human fetus. Neuroscience & Biobehavioral Reviews, 37(9, Part B), 2220–2232. Source link
Barker, D. J. (1990). The fetal and infant origins of adult disease. BMJ: British Medical Journal, 301(6761), 1111.
Barr, R. G., Rivara, F. P., Barr, M., Cummings, P., Taylor, J., Lengua, L. J., & Meredith-Benitz, E. (2009). Effectiveness of educational materials designed to change knowledge and behaviors regarding crying and shaken-baby syndrome in mothers of newborns: A randomized, controlled trial. Pediatrics, 123(3), 972. doi:10.1542/peds.2008-0908
Blackmore, E. R., Rubinow, D. R., O’Connor, T. G., Liu, X., Tang, W., Craddock, N., & Jones, I. (2013). Reproductive outcomes and risk of subsequent illness in women diagnosed with postpartum psychosis. Bipolar Disorders, 15(4), 394–404.
Brunst, K. J., Sanchez Guerra, M., Gennings, C., Hacker, M., Jara, C., Bosquet Enlow, M., … Wright, R. J. (2017). Maternal lifetime stress andprenatal psychological functioning and decreased placental mitochondrial DNA copy number in the PRISM Study. American Journal of Epidemiology, 186(11), 1227–1236.
Busnel, M. C., Fifer, W., Granier-Deferre, C., Lecuyer, R., Michel, G., Moon, C., …Spence, M. (2017). Tony DeCasper, the man who changed contemporary views on human fetal cognitive abilities. Developmental Psychobiology, 59(1), 135–139. doi:10.1002/dev.21478
Cao, X., Laplante, D. P., Brunet, A., Ciampi, A., & King, S. (2014). Prenatal maternal stress affects motor function in 5½-year-old children: Project Ice Storm. Developmental Psychobiology, 56(1), 117–125. doi:10.1002/dev.21085
Carnegie Hall Lullaby Project. (2011). Source Link
Cenit, M. C., Sanz, Y., & Codoner-Franch, P. (2017). Influence of gut microbiota on neuropsychiatric disorders. World Journal of Gastroenterology, 23(30), 5486–5498. doi:10.3748/wjg.v23.i30.5486
Cohen, S., Tyrrell, D. A., & Smith, A. P. (1991). Psychological stress and susceptibility to the common cold. New England Journal of Medicine, 325(9), 606–612.
Culhane, J. F., Rauh, V., McCollum, K. F., Hogan, V. K., Agnew, K., & Wadhwa, P. D. (2001). Maternal stress is associated with bacterial vaginosis in human pregnancy. Maternal and Child Health Journal, 5(2), 127–134.
DiPietro, J. A., Costigan, K. A., C., Hilton, S. C., & Pressman, E. K. (1999). Effects of socioeconomic status and psycosocial stress on the development of the fetus. Annals New York Academy of Sciences, 356–358.
DiPietro, J. A., Hodgson, D. M., Costigan, K. A., & Hilton, S. C. (1996). Fetal neurobehavioral development. Child Development, 67, 2553–2567.
Eckenrode, J., Campa, M., Luckey, D. W., Henderson, C. R., Cole, R., Kitzman, H., … Olds, D. (2010). Long-term effects of prenatal and infancy nurse home visitation on the life course of youths: 19-year follow-up of a randomized trial. Archives of Pediatrics & Adolescent Medicine, 164(1), 9–15.
Forrester, S., Jacobs, D., Zmora, R., Schreiner, P., Roger, V., & Kiefe, C. I. (2018). Racial differences in weathering and its associations with psychosocial stress: The CARDIA study. SSM-Population Health.
Fraiberg, S. (1995). Ghosts in the nursery: A psychoanalytic approach to the problems of impaired mother–infant relationships. In Assessment and therapy of disturbances in infancy (pp. 164–221). Northvale, New Jersey: Aronson.
Fraiberg, S., Adelson, E., & Shapiro, V. (2003). Ghosts in the nursery: A psychoanalytic approach to the problems of impaired infant-mother relationships. In J. Raphael-Leff (Ed.), Parent-Infant Psychodynamics: Wild things, mirrors and ghosts, 87, 117.
Galinsky, E. (1987). The six stages of parenthood. Boston, MA: Addison-Wesly.
Glombik, K., Stachowicz, A., Slusarczyk, J., Trojan, E., Budziszewska, B., Suski, M., … Basta-Kaim, A. (2015). Maternal stress predicts altered biogenesis and the profile of mitochondrial proteins in the frontal cortex and hippocampus of adult offspring rats. Psychoneuroendocrinology, 60, 151–162. doi:10.1016/j. psyneuen.2015.06.015
Gustafsson, H. C., Goodman, S. H., Feng, T., Choi, J., Lee, S., Newport, D. J., … Monk, C. (2018). Major depressive disorder during pregnancy: Psychiatric medications have minimal effects on the fetus and infant yet development is compromised. Development and Psychopathology, 30(3), 773–785. doi:10.1017/S0954579418000639
Hackett, R. A., & Steptoe, A. (2017). Type 2 diabetes mellitus and psychological stress—a modifiable risk factor. Nature Reviews Endocrinology, 13(9), 547—560.
Horsch, A., Kang, J. S., Vial, Y., Ehlert, U., Borghini, A., Marques-Vidal, P., … Puder, J. J. (2016). Stress exposure and psychological stress responses are related to glucose concentrations during pregnancy. British Journal of Health Psychology, 21(3), 712–729.
Lambertini, L., Chen, J., & Nomura, Y. (2015). Mitochondrial gene expression profiles are associated with maternal psychosocial stress in pregnancy and infant temperament. PLoS One, 10(9), e0138929
Laplante, D. P., Brunet, A., & King, S. (2016). The effects of maternal stress and illness during pregnancy on infant temperament: Project Ice Storm. Pediatric Research, 79(1–1), 107–113. doi:10.1038/pr.2015.177
Liang, F., Diao, L., Liu, J., Jiang, N., Zhang, J., Wang, H., … Ma, D. (2014). Paternal ethanol exposure and behavioral abnormities in offspring: Associated alterations in imprinted gene methylation. Neuropharmacology, 81, 126–133.
Lieberman, A. F., Padron, E., Van Horn, P., & Harris, W. W. (2005). Angels in the nursery: The intergenerational transmission of benevolent parental influences. Infant Mental Health Journal, 26(6), 504–520.
Lima-Ojeda, J. M., Rupprecht, R., & Baghai, T. C. (2017). “I am I and my bacterial circumstances”: Linking gut microbiome, neurodevelopment, and depression. Frontiers in Psychiatry, 8, 153. doi:10.3389/fpsyt.2017.00153
Loughnan, S. A., Sie, A., Hobbs, M. J., Joubert, A. E., Smith, J., Haskelberg, H., … Milgrom, J. (2019). A randomized controlled trial of “MUMentum Pregnancy”: Internet-delivered cognitive behavioral therapy program for antenatal anxiety and depression. Journal of Affective Disorders, 243, 381–390.
Marx, C. E., Jarskog, L. F., Lauder, J. M., Lieberman, J. A., & Gilmore, J. H. (2001). Cytokine effects on cortical neuron MAP-2 immunoreactivity: Implications for schizophrenia. Biological Psychiatry, 50(10), 743–749.
Meyer, L. E., & Erler, T. (2011). Swaddling: A traditional care method rediscovered. World Journal of Pediatrics, 7(2), 155–160. doi:10.1007/s12519-011-0268-6
Monk, C., Feng, T., Lee, S., Krupska, I., Champagne, F. A., & Tycko, B. (2016). Distress during pregnancy: Epigenetic regulation of placenta glucocorticoidrelated genes and fetal neurobehavior. American Journal of Psychiatry, 173(7), 705–713.
Monk, C., Fifer, W. P., Myers, M. M., Bagiella, E., Duong, J. K., Chen, I. S., … Altincatal, A. (2010). Effects of maternal breathing rate, psychiatric status, and cortisol on fetal heart rate. Developmental Psychobiology, 53(3), 221–233.. doi:10.1002/dev.20513
Monk, C., Fifer, W. P., Myers, M. M., Sloan, R. P., Trien, L., & Hurtado, A. (2000). Maternal stress responses and anxiety during pregnancy: Effects on fetal heart rate. Developmental Psychobiology, 36(1), 67–77.
Monk, C., Myers, M. M., Sloan, R. P., Werner, L., Jeon, J., Tager, F., & Fifer, W. P. (2004). Fetal heart rate reactivity differs by women’s psychiatric status: An early marker for developmental risk? Journal of the American Academy of Child and Adolescent Psychiatry, 43(3), 283–290.
Moon, C. M., & Fifer, W. P. (2000). Evidence of transnatal auditory learning. Journal of Perinatology, 20(8 Pt 2), S37–44.
O’Connor, E., Senger, C. A., Henninger, M. L., Coppola, E., & Gaynes, B. N. (2019). Interventions to prevent perinatal depression: Evidence report and systematic review for the US Preventive Services Task Force. JAMA, 321(6), 588–601. doi:10.1001/jama.2018.20865
Olds, D. L., Kitzman, H., Cole, R., Robinson, J., Sidora, K., Luckey, D. W., … Holmberg, J. (2004). Effects of nurse home-visiting on maternal life course and child development: Age 6 follow-up results of a randomized trial. Pediatrics, 114(6), 1550–1559.
Olds, D. L., Robinson, J., Pettitt, L., Luckey, D. W., Holmberg, J., Ng, R. K., … Henderson, C. R. (2004). Effects of home visits by paraprofessionals and by nurses: Age 4 follow-up results of a randomized trial. Pediatrics, 114(6), 1560–1568.
Pennebaker, J. W. (2000). Telling stories: The health benefits of narrative. Literature and Medicine, 19(1), 3–18.
Pinilla, T., & Birch, L. L. (1993). Help me make it through the night: Behavioral entrainment of breast-fed infants’ sleep patterns. Pediatrics, 91(2), 436–444.
Posner, J., Cha, J., Roy, A., Peterson, B., Bansal, R., Gustafsson, H., … Monk, C. (2016). Alterations in amygdala–prefrontal circuits in infants exposed to prenatal maternal depression. Translational Psychiatry, 6(11), e935.
Pressman, E., DiPietro, J., Costigan, K., Shupe, A., & Johnson, T. (1998). Fetal neurobehavioral development: Associations with socioeconomic class and fetal sex. Developmental Psychobiology, 33(1), 79–91.
Rudolph, M. D., Graham, A. M., Feczko, E., Miranda-Dominguez, O., Rasmussen, J. M., Nardos, R., … Fair, D. A. (2018). Maternal IL-6 during pregnancy can be estimated from newborn brain connectivity and predicts future working memory in offspring. Nature Neuroscience, 21(5), 765–772. doi:10.1038/s41593-018-0128-y
Sacks, K. N., Friger, M., Shoham-Vardi, I., Abokaf, H., Spiegel, E., Sergienko, R., … Sheiner, E. (2016). Prenatal exposure to gestational diabetes mellitus as an independent risk factor for long-term neuropsychiatric morbidity of the offspring. American Journal of Obstetrics & Gynecology, 215(3), 380, e381–380.e387.
Sánchez-Villegas, A., Toledo, E., de Irala, J., Ruiz-Canela, M., Pla-Vidal, J., & Martínez-González, M. A. (2012). Fast-food and commercial baked goods consumption and the risk of depression. Public Health Nutrition, 15(3), 424–432.
Sánchez-Villegas, A., Verberne, L., De Irala, J., Ruíz-Canela, M., Toledo, E., Serra-Majem, L., & Martínez-González, M. A. (2011). Dietary fat intake and the risk of depression: The SUN Project. PLoS One, 6(1), e16268
Sandman, C. A., Wadhwa, P. D., Dunkel–Schetter, C., Chicz–DeMet, A., Belman, J., Porto, M., … Crinella, F. M. (1994). Psychobiological influences of stress and HPA regulation on the human fetus and infant birth outcomes. Annals of the New York Academy of Sciences, 739, 198–210.
Slade, A., Sadler, L., De Dios-Kenn, C., Webb, D., Currier-Ezepchick, J., & Mayes, L. (2005). Minding the baby a reflective parenting program. Psychoanalytic Study of the Child, 60, 74–100.
Spann, M. N., Monk, C., Scheinost, D., & Peterson, B. S. (2018). Maternal immune activation during the third trimester is associated with neonatal functional connectivity of the salience network and fetal to toddler behavior. The Journal of Neuroscience, 38(11), 2877–2886. doi:10.1523/ jneurosci.2272-17.2018
St. James-Roberts, I., Sleep, J., Morris, S., Owen, C., & Gillham, P. (2001). Use of a behavioural programme in the first 3 months to prevent infant crying and sleeping problems. Journal of Paediatrics and Child Health, 37(3), 289–297.
Thayer, Z. M., Wilson, M. A., Kim, A. W., & Jaeggi, A. V. (2018). Impact of prenatal stress on offspring glucocorticoid levels: A phylogenetic meta-analysis across 14 vertebrate species. Science Reports, 8(1), 4942. doi:10.1038/s41598-018-23169-w
van den Bergh, B. R. H., van den Heuvel, M. I., Lahti, M., Braeken, M., de Rooij, S. R., Entringer, S., … Schwab, M. (2017). Prenatal developmental origins of behavior and mental health: The influence of maternal stress in pregnancy. Neuroscience & Biobehavioral Reviews. doi:10.1016/j.neubiorev.2017.07.003
van Sleuwen, B. E., Engelberts, A. C., Boere-Boonekamp, M. M., Kuis, W., Schulpen, T. W., & L’Hoir, M. P. (2007). Swaddling: A systematic review. Pediatrics, 120(4), e1097–1106. doi:10.1542/peds.2006-2083
Vermeulen, E., Stronks, K., Snijder, M. B., Schene, A. H., Lok, A., de Vries, J. H., … Nicolaou, M. (2017). A combined high-sugar and high-saturated-fat dietary pattern is associated with more depressive symptoms in a multi-ethnic population: The HELIUS (Healthy Life in an Urban Setting) study. Public Health Nutrition, 20(13), 2374–2382.
Werner, A., Myers, M. M., Fifer, W. P., Cheng, B., Fang, Y., Allen, R., & Monk, C. (2007). Prenatal predictors of infant temperament. Developmental Psychobiology, 49, 474–484.
Xiang, A. H., Wang, X., Martinez, M. P., Walthall, J. C., Curry, E. S., Page, K., … Getahun, D. (2015). Association of maternal diabetes with autism in offspring. JAMA, 313(14), 1425–1434.
Zhang, S., Ding, Z., Liu, H., Chen, Z., Wu, J., Zhang, Y., & Yu, Y. (2013). Association between mental stress and gestational hypertension/preeclampsia: A metaanalysis. Obstetrical & Gynecological Survey, 68(12), 825–834.




