Julia Yeary, Cross Plains, Wisconsin
Vincent C. Smith, Boston Medical Center, Boston, Massachusetts; Boston University Chobanian & Avedisian School of Medicine
Abstract
There is an increased recognition for the need to have national guidance for discharge preparation and transition planning for infants in neonatal intensive care units (NICUs) as a key component of family-centered NICU care (Vohr, 2022). As babies transition home, many still have special care needs. The National Perinatal Association recognized this need and convened a working group to create national guidelines reflecting the best available evidence from across disciplines. Recently published, the Interdisciplinary Guidelines and Recommendations for NICU Discharge Preparation and Transition Planning (Smith et al., 2002b) provide clear and concise guidance that is both general and adaptable while also being specific and actionable. The Discharge Guidelines promote starting where the family is, recognizing each family’s unique make-up, values, beliefs, and cultural norms.
Malia was worried. Baby “H” still hadn’t had any visitors. He was born at just 28 weeks gestation, and now lay in the neonatal intensive care unit (NICU) with its bright lights, beeps from machines, constant buzz of movement, and frequent alarms. Multiple wires and tubes were connected to his tiny body, his eyes taped closed. At just 5 days old, he had a tough journey ahead of him, but he looked like quite the fighter! Malia checked the team notes and read that Baby H’s mother, Edeline, is a 15-year-old who is an unaccompanied minor child in a contracted group home, with the Office of Refugee Resettlement designated as legal authority for the teen mother. As the NICU social worker, it was Malia’s job to support both the family and the unit in ensuring Baby H had a home to go to where his medical needs, his physical needs, and his social–emotional needs would be met. Malia saw that Edeline spoke only Creole, a dialect in Haiti where Edeline grew up. Malia was worried. Edeline needed to be here with her baby, forming that important connection with her son. She wondered where she could find a medical translator fluent in Creole, which was not a common language for patients in this hospital. She wondered if the group home planned on Baby H and Edeline living there together, or if there were any other plans? And how often could they arrange for Edeline to be with her son? She reached for the phone to contact the group home.
With so much going on medically in a NICU, it is easy to lose sight of the nonmedical needs of the infants. The American Academy of Pediatrics recommends the transition from the NICU to home occurs when an infant achieves physiological stability and there is an active program for parental involvement and preparation for care of the infant at home (American Academy of Pediatrics Committee on Fetus and Newborn, 2008). With the uniqueness of each individual baby and family, ensuring the needs of each are met can feel messy and uncoordinated. Before a baby is discharged, care should be taken to ensure that the caregivers have received the necessary teaching and training required to care for baby; a comprehensive discharge plan is in place; and there have been arrangements for outpatient follow-up in a medical home familiar with the care of infants who have been in the NICU. The baby’s health is at stake, so caregivers must be able to demonstrate mastery of essential knowledge and skills. The transition from hospital to home requires coordination between family caregivers, the medical team, and community supports such as early intervention programs and social support programs.
Discharge Readiness and Discharge Preparation
NICU discharge readiness is the attainment of technical skills and knowledge, emotional comfort, and confidence with infant care by the infant’s primary caregivers at the time of discharge. NICU discharge preparation is the process of facilitating discharge readiness to successfully make the transition from the NICU to home. Discharge readiness is the desired outcome, discharge preparation is the process. (Smith et al., 2013, pp. 2–3)
The National Perinatal Association (NPA) recognized that while there was clear guidance on what constitutes physiological maturity in the infant, there was only limited guidance about what should be included in a comprehensive discharge planning program for a family. In response to the need for national guidelines for NICU discharge preparation and transition planning, NPA convened a workgroup (see Box 1) with the goal of creating comprehensive guidelines that reflect the best available evidence from across disciplines and informed by families’ experiences. They knew a comprehensive guide would include:
• well-defined discharge teaching philosophy,
• structured education program,
• defined curriculum,
• family assessment of discharge readiness, and
• process for the transition of care to a medical home.
Box 1. Committee, Workgroup, and Expert Contributors
Steering Committee
Vincent C. Smith, MD, MPH (Chair)
Erin Armknecht
Patty Briges, MSW, LCSW
Joy Browne, PhD, PCNS, IMH-E(IV) Jenene Craig, PhD, MBA, OTR/L
Brigitte C. Desport, DPS, OTR/L, BCP, ATP Erika Goyer
Cristal Grogan
Andrea Werner Insoft, LICSW, ACSW
Kristy Love
Cheryl Milford, EdS
Steve Richardson
Tiffany Willis, PsyD
Julia Yeary, LCSW, IMH-E (IV, Policy and Clinical)
Interdisciplinary Guidelines and Recommendations Development Workgroup
Vincent C. Smith, MD, MPH
Erin Armknecht
Patty Briges, MSW, LCSW
Joy Browne, PhD, PCNS, IMH-E(IV)
Jenene Craig, PhD, MBA, OTR/L
Brigitte C. Desport, DPS, OTR/L, BCP, ATP
Heidi Gates, RN
Erika Goyer
Cristal Grogan
Andrea Werner Insoft, LICSW, ACSW
Carol Jaeger, DNP, RN
Judi Kellkamp, PT
Kristy Love
Cheryl Milford, EdS
Trudi N. Murch, PhD, CCC-SLP
Heather Cohen Padratzik, MHA, JD
Steve Richardson
Cuyler Romeo, MDT, OTR, SCFES, CLC
Betty Vohr, MD
Tiffany Willis, PsyD
Julia Yeary, LCSW, IMH-E (IV, Policy and Clinical)
Additional Content Expert Contributors
Michael T. Hynan, PhD
Carole Kenner, PhD, RN, FAAN Jonatha S. Litt, MD, MPH, ScD Nicole Lomerson, MPH
Molly Fraust Wylie
NPA Staff
Erika Goyer Kristy Love
The workgroup began the process by completing an environmental scan that reviewed existing standards for NICU discharge preparation and planning. After reviewing existing guidelines and conducting a literature review, they drafted a list of evidence-informed, multidisciplinary, and consensus guidelines. They looked for differences in practices and identified gaps. Next, the workgroup convened their first summit in 2019 with 16 multidisciplinary experts representing 14 different organizations. With the experts’ input, the workgroup put together their suggested guidelines. Following this meeting, five members of the workgroup assisted with verification of evidence for each guideline and rated the level of evidence for each item. Then they were ready for a second summit.
During the second summit in 2021, NPA’s Discharge Planning workgroup was able to convene 22 multidisciplinary experts representing 19 different organizations to review the revised guidelines. As with the first summit, the group reviewed each guideline, answering the following questions:
• Is the content appropriate?
• Is the content complete or is there information missing?
• Are the recommendations appropriate, practical, and actionable?
• Are the recommendations clear and concise?
• Are the recommendations comprehensive and complete?
Following receipt of the reports from the summit, the workgroup revised and updated the draft guidelines. The Interdisciplinary Guidelines and Recommendations for NICU Discharge Preparation and Transition Planning (Discharge Guidelines; Smith et al., 2022b) should be beneficial, useful, and pertinent. The workgroup needed to provide more uniformity in discharge preparation and, consequently, reduce uncertainty and stress with the discharge preparation and transition planning process. They needed to help professionals meet the family where they were—not where they wanted them to be. The workgroup finalized all of the guidelines and the Discharge Guidelines were published in the Journal of Perinatology in March 2022.
A Holistic Approach
The Discharge Guidelines go beyond the medical needs of the newborn. They help teams to focus on the newborns in their care and those babies’ caregivers more holistically. The foundation of all the guidelines rests in existing literature, practice, and policy. The workgroup also had direct input from families with lived experiences to inform recommendations. The guidelines are divided in the following sections:
• basic information
• anticipatory guidance
• family and home needs assessment
• transfer and coordination of care
• other important considerations
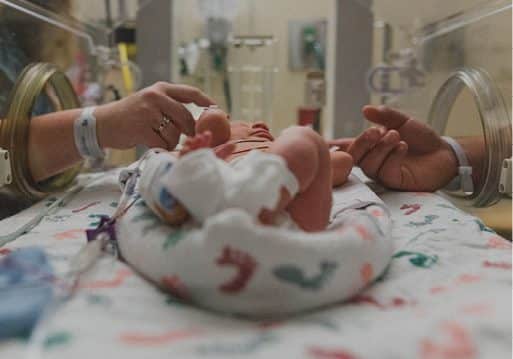
The Discharge Guidelines help teams to focus on the newborns in their care and those babies’ caregivers more holistically. Photo: Shutterstock/Jesica Montgomery
Each section includes a brief introduction, the guidelines in table format, followed by further descriptors and guidance as needed. Guidance is offered in clear, easy-to-read tables, with references offered if the reader would like to know more about the evidence about the inclusion of the guideline.
Addressing Diversity, Equity, Inclusion, Accessibility, and Belonging
When considering families like the one in the earlier vignette, it is important to make sure the discharge preparation can accommodate special circumstances, such as the birth mother being a minor who resides in a group home, and having, in this case, no understanding of English. The Discharge Guidelines include detailed guidance in other important considerations including working with:
• families with limited English proficiency
• military families
• LGBTQIA+-headed families
• parents with disabilities
• families with distinct cultural and/or philosophical expectations
The Discharge Guidelines set a standard of being intentional in addressing diversity, equity, inclusion, accessibility, and belonging. The Discharge Guidelines promote supporting caregivers of NICU patients so they feel safe and secure with the care their baby and they receive while connected to the NICU (Smith et al., 2022a).
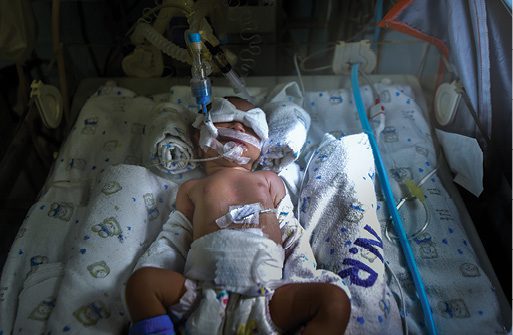
Having a baby with serious medical concerns, including preterm birth, can be very stressful for a family, even traumatic. Photo: Shutterstock/Charlie Chulapornsiri
Malia ensured she had the hospital’s new release of information forms as she got ready for Edeline, the mother of Baby H, to visit with the staff from the group home. Recently, the hospital’s legal department had reviewed all the NICU release of information forms to allow for special circumstances such as HIPAA medical information release based on needs of the family rather than biological relationships. She knew this would allow her to create a working relationship with the group home as well as with Edeline.
This change to legal forms to allow for different family and caregiver configurations had especially been important recently in another scenario involving Baby T. Baby T’s biological mother, Sasha, and co-parent, Nara, were not married legally, but were committed to raising their son together. They had been through the in vitro fertilization process together. Before the change in their processes, the staff would have had difficulty providing Nara the support she needed as a co-parent. This process change had really simplified matters while supporting the best interest of the family’s need to ensure confidentiality of health information.
Applying the Discharge Guidelines encourages organizations to review processes and policies to ensure they are family-friendly. It is vital to support the strong connection between baby and parent. Having a baby with serious medical concerns, including preterm birth, can be very stressful for a family, even traumatic. Removing barriers to families receiving the support they want is critical. The Discharge Guidelines include the recommendation that a key element of discharge preparation involves asking the primary caregivers if and which additional support persons they would like to participate in the discharge preparation. These are the people who will be supporting the baby and baby’s caregivers in the important days following discharge. NICU staff must ask if any of these support persons should be included in the teaching of necessary caregiving skills. In the case of Baby H and Edeline, this would be key adults who support Edeline, even if they are not legally part of the family unit. This group could include family elders, religious leaders, or ethnic leaders, even though those people are not typically included when thinking of “caregiver.” In Baby T’s case, discharge preparation would be acknowledging their family structure and respecting parental authority for both parents.
A Variety of Teaching Methods
In teaching the family the essential knowledge and skills needed to care for the baby, it’s valuable to consider using multiple methods of teaching. Even with English-proficient families, or with competent medical translators, the information can feel overwhelming and scary. Families may wonder: “What if a procedure isn’t done correctly? What if there is a problem?” The NICU team wants the caregivers to feel comfortable, feel confident, and be competent. The use of pictures to demonstrate needed steps, as well as allowing caregivers to video record the process, can make a huge difference in helping caregivers remember the necessary steps of caring for their medically fragile infant. In an emergency, NICU teams may need to use family members for translations to the family’s preferred language, but it is preferred practice to use certified medical translators to be certain the family understands fully the information being shared. Professional translation, along with use of nonwritten forms and instructions, helps the family review needed steps whenever they desire, rather than relying on only the typical written literature. The Discharge Guidelines explain in detail considerations when working with families with limited English proficiency. These non-literary based teaching tools are also helpful when supporting caregivers with intellectual disabilities.
Multidisciplinary Support and Collaboration
NICU teams may bring in other members of the hospital team as needed to support optimal instruction and planning, and to think about making caregiving easier when baby gets home.
Mandy, a discharge planner for the NICU team, noticed the teaching room didn’t have much space to maneuver. Baby Z’s dad was present but basically stuck at the doorway because his wheelchair didn’t fit around the table and chairs in the room. She immediately checked to see if the larger classroom was available and moved the teaching to that location to help Baby Z’s dad feel more comfortable. She asked the family how they felt about asking the Occupational Therapy Department to do a consult with them to help adapt their home so they can be ready for both parents to be fully involved caregivers for Baby Z.
The Discharge Guidelines also state personnel to whom families are referred should have the specialized training and knowledge needed to support the newborn and their family with any identified needs. For example, refer a new lactating mother who has physical challenges to a lactation consultant who has experience working with individuals with physical disabilities. Growing a community of resources available to the NICU team’s families is key. NICU teams may need to think about how they collaborate with the agencies within their area of service. Creating strong relationships can be very helpful, especially with those agencies providing services used most often such as early intervention programs. Consider bringing community resource personnel into the hospital for the caregivers to meet before discharge. Sometimes their knowledge of communities and their cultural norms can be very informative, and they may be able to suggest ways to address possible barriers for care.
LaKrisha, the service coordinator for the local early intervention agency, was so warm as she met Baby D’s family. Nancy, the NICU discharge coordinator, and Henry, the team’s social worker, were surprised by one question LaKrisha asked the family: Where did they want to meet for their home visits? Nancy and Henry assumed the visits would be in the family’s home. LaKrisha knew the area where the family lived, and she suspected the home had multiple families living in a small space. The family shared they would feel more comfortable with meeting at the library, just a block away. There just wasn’t space for a private visit at home. And, notably, most of the other people at their home didn’t feel comfortable with strangers in the house, because they were concerned about immigration services. The family was very appreciative that this option was even possible. LaKrisha shared later that providing alternate places to meet improved family’s attendance at “home” visits. The early intervention agency used the library, parks, shopping centers, homes of relatives, community centers, or anywhere the family felt comfortable.
Of course, creating a comprehensive discharge preparation and transition planning program that would fit into every unique NICU and hospital setting is not possible. The work-group for the Discharge Guidelines took this into consideration, and instead focused on recommendations that were both general and adaptable while also being specific and actionable. Implementation of these Discharge Guidelines will be informed by the distinctive characteristics of the NICU team, including the team make-up, the community served, and the resources available.
Comprehensive, Consistent, and Clear
When preparing for a baby to be discharged from the NICU to home, the NICU team must start by setting clear criteria for what each family system and infant need to accomplish to be ready for the transition. Helping families to understand the fluidity of the process is a part of this. At a moment’s notice, something can change. Everything will shift in response to the medical needs of the infant. It can be very difficult for families to deal with the roller-coaster emotions that accompany these shifts. Clarity in communicating this to families is an important part of earning their trust. The entire team needs to ensure there is consistent messaging. The Discharge Guidelines include suggestions for team communication to assist with this (Smith et al., 2022a).
Discharge preparation and transition planning must go beyond instructions on how to perform caregiving tasks. The NICU team must recognize caregivers are adjusting to what it means to parent a medically fragile child. A comprehensive discharge plan must address the social and emotional needs of the family system and strengthen access to supports that will help families to be fully prepared to welcome and care for their new child. The Interdisciplinary Guidelines and Recommendations for NICU Discharge Preparation and Transition Planning is a tool all NICU teams, as well as agencies that support medically fragile infants, can use to support parents in being confident, competent, and loving in caring for their child.
Author Bios
Julia Yeary, LCSW, IMH-E®, retired from ZERO TO THREE and now provides infant and early childhood mental health consultation. She was a part of the Discharge Guidelines Steering Committee and assisted with editing of the guidelines. She resides in Cross Plains, WI.
Vincent C. Smith, MD, MPH, is division chief of newborn medicine at Boston Medical Center and professor of pediatrics at Boston University Chobanian & Avedisian School of Medicine. He is a former member of the National Perinatal Association Board of Directors and the chair of the Discharge Guidelines Steering Committee. Dr. Smith is a proud ZERO TO THREE Graduate Fellow.
References
American Academy of Pediatrics Committee on Fetus and Newborn. (2008). Hospital discharge of the high-risk neonate. Pediatrics, 122(5), 1119–1126.
Smith, V. C., Hwang, S. S., Dukhovny, D., Young, S., & Pursley, D. M. (2013). Neonatal intensive care unit discharge preparation, family readiness and infant outcomes: Connecting the dots. Journal of Perinatology, 33(6), 415–421.
Smith, V. C., Love, K., & Goyer, E. (2022a). Correction to: NICU discharge preparation and transition planning: Guidelines and recommendations. Journal of Perinatology, 42(Suppl 1), 25. doi: 10.1038/s41372-022-01371-z. Erratum for Journal of Perinatology, 42(Suppl 1), 7–1. PMID: 35354943; PMCID: PMC9010293.
Smith, V. C., Love, K., & Goyer, E. (2022b). NICU discharge preparation
and transition planning: Guidelines and recommendations. Journal of Perinatology, 42, 7–21. www.nature.com/articles/s41372-022-01313-9
Vohr, B. R. (2022). NICU discharge preparation and transition planning: Editorial. Journal of Perinatology, 42(Suppl 1), 1–2. doi: 10.1038/s41372-022- 01310-y. Erratum in Journal of Perinatology, Apr 1. PMID: 35165373; PMCID: PMC9010287.



