What the report says:
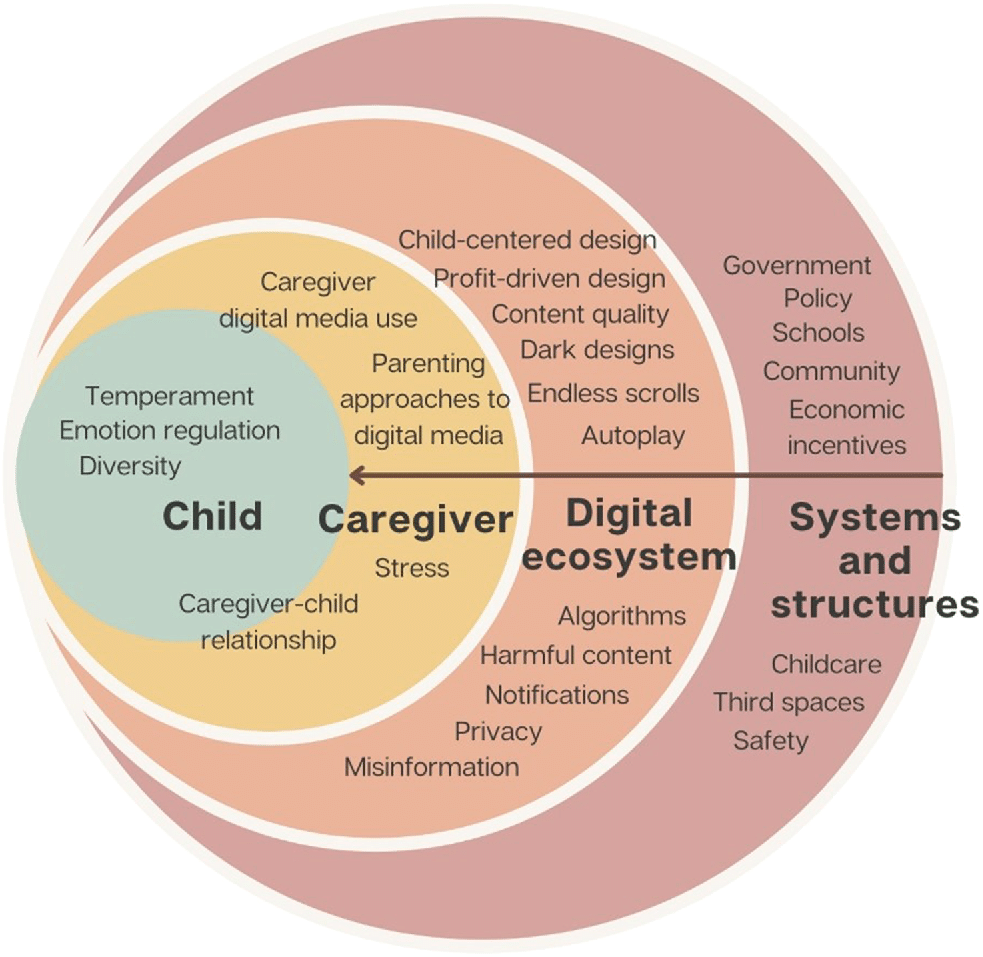
The American Academy of Pediatrics’ report on digital ecosystems describes how today’s media environment is intentionally designed to capture and sustain user attention, with implications that begin early in childhood. The report emphasizes that children are growing up in a digital context shaped by algorithm-driven, highly engaging, and often fast-paced content that can influence attention, behavior, and development.
For young children, whose cognitive and self-regulation systems are still developing, this environment can make it harder to disengage from screens, sustain attention in non-digital contexts, and build foundational skills through real-world interaction. The report underscores that early and frequent exposure to these design features, especially without adult support, may shape habits, expectations, and developmental pathways over time.
Rebecca’s thoughts:
This research reinforces something we have long understood about early childhood development. Young children learn best through relationships. Screens can be a tool, but they are not a substitute for the back-and-forth interactions that build language, thinking, and emotional skills in the earliest years.
Most importantly, children need opportunities to practice resilience as they encounter normal stressors in daily life. It’s the block tower that fell, it’s waiting in line with a parent at the supermarket, it’s disappointment that the bakery is out of donuts with sprinkles on top. If children consistently use screen media to cope with these everyday annoyances and stressors, they may not get the practice they need to develop skills like grit, resilience, and regulation that they’ll need later on in school and life.
What is especially striking is taking a moment to consider not just how much media young children are using, but what kind. Much of children’s media time is now spent with short-form entertainment content which is increasingly consumed on mobile devices, often used alone or as part of daily routines. That matters. Research tells us that both the media content and how it’s delivered will shape child outcomes. Educational content, used together with a caregiver, can support learning. But fast-paced, short-form entertainment (noneducational) media used solo does not offer those same benefits. In fact, short-form media (like “AI slop”) can be of shockingly low quality and expose children to content and ads that are not age-appropriate at best, and disturbing or harmful at worst. Overall, high screen use can easily crowd out the kinds of play and interaction that young children need most.
As Dr. Jenny Radesky explains in our recent article, the attention economy adds an important layer to this conversation. Many of today’s digital experiences are designed to capture and hold attention so that viewers stay with a video long enough to receive an ad. The goal is not to support development. Young children are specifically vulnerable to this type of content. Their brains are wiring based on early experiences. If they are consistently exposed to short-form media content, that can mean more fragmented attention, more difficulty with self-regulation, and fewer opportunities for sustained, meaningful interaction. Supporting families today means helping them navigate this environment with intention and balance, while keeping relationships at the center of early development.



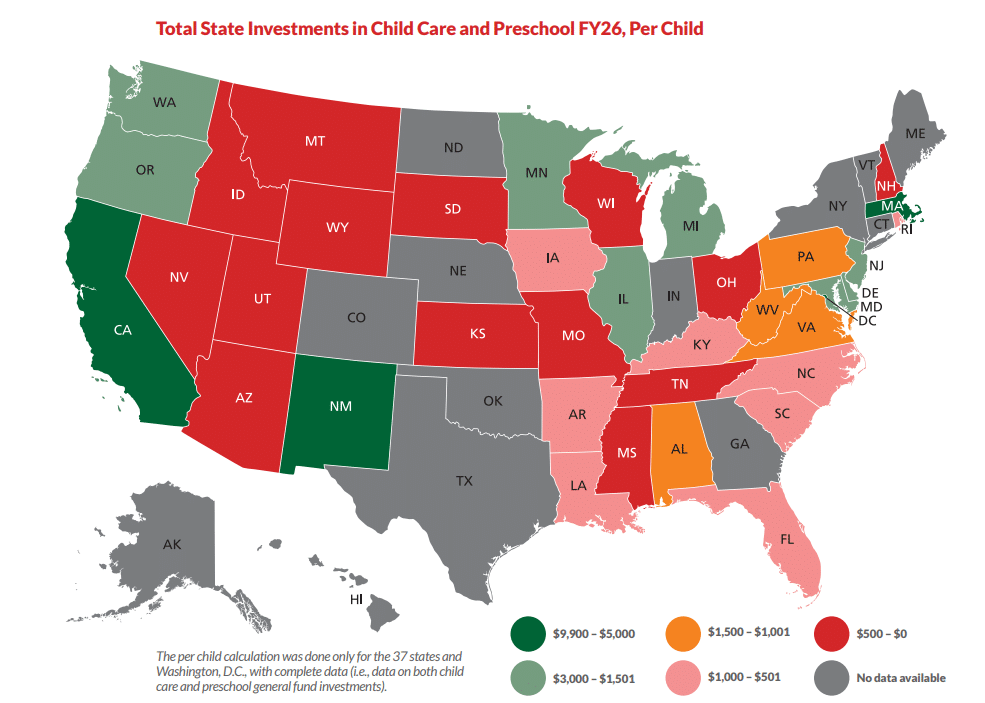



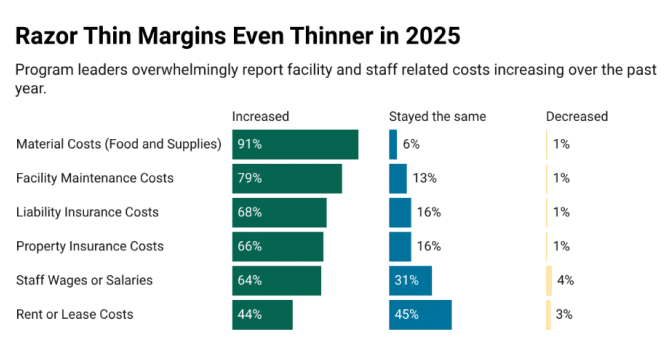
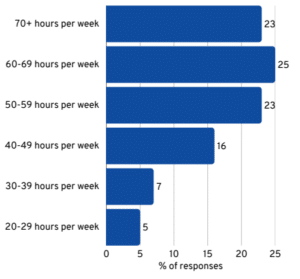
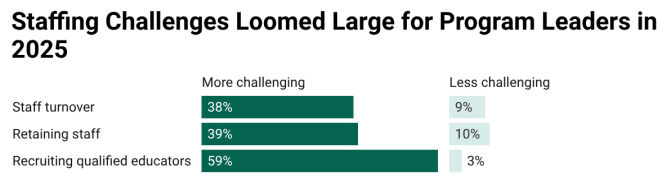


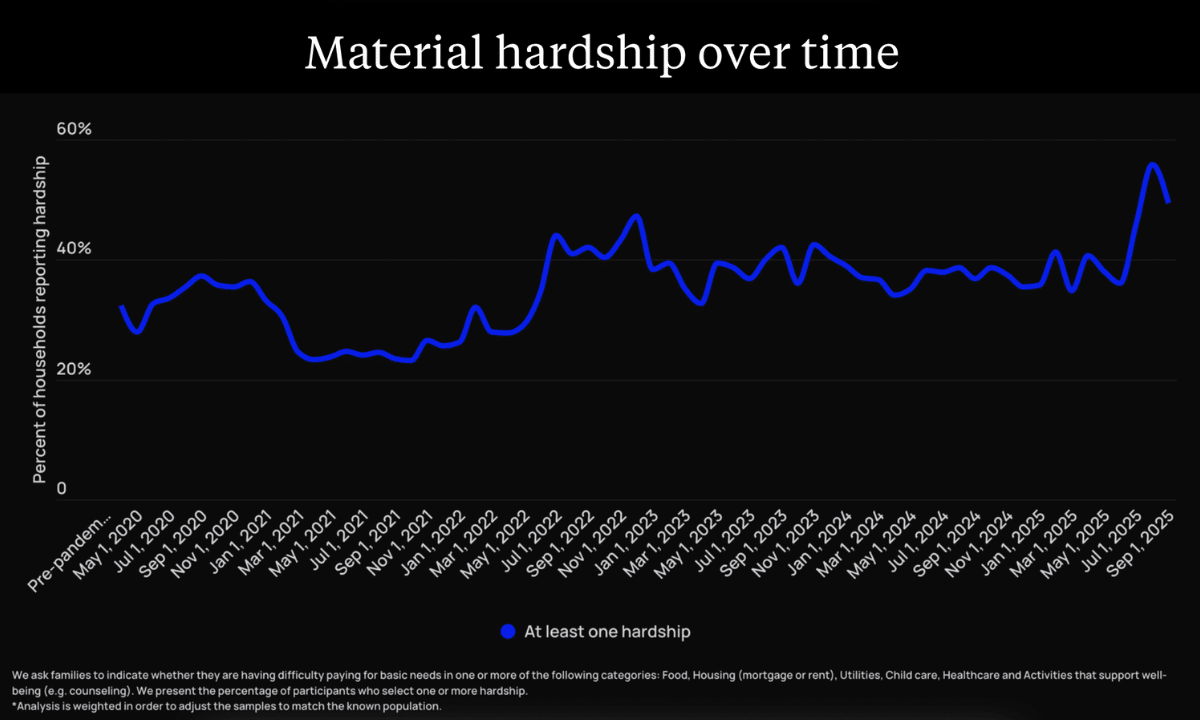
 A recent Seattle Times article focuses on the School House Connection report,
A recent Seattle Times article focuses on the School House Connection report, 

 Phil’s take:
Phil’s take:

 What the research says:
This study examined whether recorded maternal speech could influence brain development in very preterm infants cared for in the neonatal intensive care unit (NICU). Researchers played recordings of mothers reading aloud to their babies for several hours each night over multiple weeks. MRI scans taken near term-equivalent age showed that infants exposed to these recordings had more mature development in the left arcuate fasciculus, a brain pathway critical for speech and language.
The findings suggest that consistent exposure to human speech, even in the earliest stages of life, may help strengthen neural connections that support later language development.
Mike’s take:
We know that nurturing relationships and low parental stress are essential to healthy child development,
What the research says:
This study examined whether recorded maternal speech could influence brain development in very preterm infants cared for in the neonatal intensive care unit (NICU). Researchers played recordings of mothers reading aloud to their babies for several hours each night over multiple weeks. MRI scans taken near term-equivalent age showed that infants exposed to these recordings had more mature development in the left arcuate fasciculus, a brain pathway critical for speech and language.
The findings suggest that consistent exposure to human speech, even in the earliest stages of life, may help strengthen neural connections that support later language development.
Mike’s take:
We know that nurturing relationships and low parental stress are essential to healthy child development,