Maria Kroupina and Kathryn Elison, University of Minnesota

Abstract
Children from birth to 3 years old with complex medical needs often experience psychological issues, but there are limited services and supports to meet their needs. To bridge this gap, the authors created the Pediatric Birth to Three Clinic and Early Childhood Mental Health Program at the University of Minnesota. They describe the toxic stress framework of their approach and the relationship-based and trauma-informed treatment modalities used to support the young children and their families in their care.
The Pediatric Birth to Three Clinic and Early Childhood Mental Health Program emerged from combining knowledge from two areas—toxic stress and early childhood mental health—and applying it in the novel context of pediatrics. Combining expertise on the impact of toxic stress on developing brains, with early intervention for children from birth to 3 years old, and a strong background in child development, we can fill a large gap in existing pediatric care. We strive to be able to identify children at risk for toxic stress and intervene at the earliest point with medically complex children.
Many pediatric services are designed to monitor children’s development or provide additional levels of support in a crisis; however, our program seeks to be preventive in nature under the best circumstances and provide direct intervention to those in need of it. We seek to join with families that have the youngest patients in the pediatric setting to support typical development in an atypical environment, improve the existing relationships between caregiver and child, and enhance the sensitivity of caregivers to their children’s behavioral cues especially under times of great stress, such as during a hospitalization. In the following sections we will review the impetus behind the creation of this novel program as well as outline how we support the youngest patients in the pediatric setting.
Toxic Stress
During the first years of life, the human brain is in its most plastic and sensitive period, making it vulnerable to environmental factors, including toxic stress. Research from human and animal models has aided researchers in proposing three different categories of stress affecting children. The first, labeled positive stress, applies to a physiological state that is mild and brief. Experiences such as getting an immunization or dealing with frustration or a child’s first day at child care could all lead to positive stress. Positive stress can actually be beneficial to children, given that it provides opportunities to learn and practice healthy methods of dealing with everyday stress. The second category of stress is tolerable stress. While similar to positive stress, these experiences are considered non-normative and present a greater magnitude of threat. Experiences such as serious illness, death of a family member, or a natural disaster would be classified as tolerable as long as they are experienced in conjunction with a supportive relationship that aids the child in coping with the stressful experience and thus reducing the physiological stress response. The third and most harmful classification is toxic stress. Toxic stress is caused by an experience(s) that produces frequent, strong, and/or prolonged activations of the body’s stress response systems in the absence of the protection of a supportive adult relationship. These types of stressors can range from child abuse to maternal depression.
Toxic stress affects metabolic systems, brain circuitry, and a child’s overall mental health. This is especially true between birth and 3 years old. Supportive relationships can protect against the impact of this stress and are classified as relationships from which a child can seek help from a caring and responsive adult who can help the child’s stress system return to baseline. These relationships are considered “buffers” because they can provide some insulation between the child and the stressful experience. While it is not always easy to identify toxic stress, it is incredibly important to do so. The effects of toxic stress experienced in early childhood can often last a lifetime (Shonkoff & Garner, 2012).
Effects of Toxic Stress
Extant research indicates that toxic stress can have both short- and long-term effects on a child. Toxic stress can lead to disturbances in the regulation of the body’s stress-sensitive systems, which results in the circulation of stress hormones becoming either chronically excessive or chronically deficient. The plasticity of the developing brain allows toxic stress to have dramatic neurological effects on children in their first 3 years of life. Early toxic stress can have the most detrimental effect on three regions of the brain. Significant early stress can trigger hypertrophy of the amygdala, a region of the brain critical in activating the physiological stress response, and result in a chronically activated stress response system (National Scientific Council on the Developing Child, 2010).
While the amygdala plays a role in turning on the physiological stress system, the hippocampus normally turns off elevated cortisol levels. Chronic stress, however, diminishes its capacity to do so. This damage to the hippocampus also impairs memory and its mood-related functions (National Scientific Council on the Developing Child, 2005/2014). The third brain region most sensitive to toxic stress is the prefrontal cortex. Elevated cortisol (a product of toxic stress) changes the connectivity in the prefrontal cortex, which in turn hinders its ability to inhibit an overactive amygdala (Boyce & Ellis, 2005). These neurological changes can have long-term effects on a child’s physiological, cognitive, and social development. An individual’s response to toxic stress will vary due to genetic predisposition; availability of supportive relationships; and the duration, intensity, timing, and context of the stressful experience.
Buffering the Impact of Toxic Stress
Although it is not yet understood how toxic stress will specifically affect individual children, extensive research findings emphasize the importance of a supportive relationship. Stress does not become toxic if children have a supportive relationship from which they can seek comfort. Children without this optimal buffering are at a much higher risk for experiencing toxic stress. Almost all children form attachment relationships with their caregivers, but the quality of these relationships can vary dramatically. Attachment relationships are driven by biological need, and they form in the first year of a child’s life. Secure attachment relationships are the most effective at protecting a child from a stressful experience and occur in the presence of consistent caregiving, when the adult has reliably been able to meet the needs of the child. Having this supportive relationship in times of stress can have a profound insulating effect on children both psychologically and biologically. In a series of studies by Gunnar and Donzella (2002), children who were exposed to stressful situations such as receiving an immunization, being approached by a loud robot, or meeting a clown did not show the expected elevated cortisol levels if they were in the company of an adult with whom they had a secure emotional relationship. Children with insecurely attached relationships who were exposed to these same conditions did show a high stress response.
Unfortunately, some children who are exposed to multiple risk factors, such as high parental stress or psychopathy, multiple foster care placements, or neglect or abuse in their family, do not form optimal attachment relationships. Children with a history of experiencing less-than-optimal buffering relationships show more self-regulation challenges, including sleep, eating, and emotion regulation issues. Children who have experienced other risk factors such as premature birth, prenatal drug exposure, or compromised health status have also been found to be more sensitive to the effects of the quality of buffering relationships.
Pediatrics Population and Toxic Stress
The earliest system that is involved in children’s lives is the health care system or hospital. The need for screening, early identification of concerns, and brief intervention are well documented (Osofsky & Lieberman, 2011; Shonkoff & Garner, 2012); however, there is a prominent gap in mental health services that begins at birth for children who are being served by the hospital system. Early childhood mental health issues tend to go unidentified due to a lack of early biomarkers and training programs that teach pediatric providers about the early biomarkers or behavioral signs of problems that can be addressed.
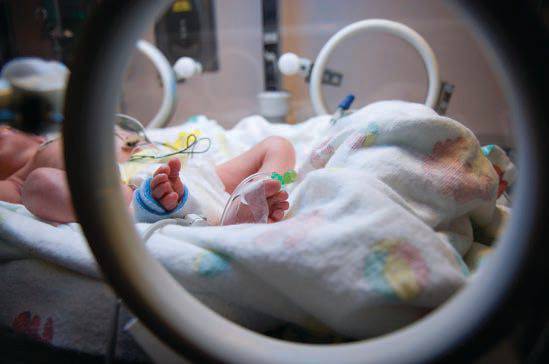
Young children who spend time in the hospital are also at unique risk for negative outcomes due to sequela of congenital or chronic health conditions that alter the course of development at both the child and systems level. Chronic illness can cause repeated exposure to stressful events such as multiple surgeries, hospitalizations, doctor visits, and blood draws. In cases when these medically compromised children also lack an effective adult buffer, each of these exposures to a stressful event has the potential to be toxic, further rewiring brain networks, altering the stress response system and placing these medically fragile children at an even higher level of increased risk for long-term negative outcomes.
Pediatric Birth to Three Clinic and Early Childhood Mental Health Program
Despite overwhelming evidence pointing to the importance of early childhood (e.g., birth to 3 years) mental health interventions in mitigating or completely preventing negative outcomes, early childhood mental health is not yet integrated within pediatric training and clinic systems in the US. Pediatricians may not always be aware of the interventions available or may believe they should wait until a child is older before making a referral. A mental health referral for children as young as 3 or 6 months may seem novel. Toxic stress, however, as identified by the American Academy of Pediatrics, poses significant risks to the health and normal development of very young children (Shonkoff & Garner, 2012). Any child who appears to be at risk for toxic stress needs to receive a referral to a specialist for treatment.
The need for referral is where the Pediatric Birth to Three Clinic and Early Childhood Mental Health Program comes in. We provide support to medical teams and families who are at unique risk for experiencing toxic stress. By creating an informed system on these areas of expertise, creating access to professionals who can intervene as needed, and supporting families where they are getting their medical care, we are better meeting the needs of these very vulnerable children.

For some pediatric patients, their home is the hospital and interventions have to be modified to be delivered in the medical context.
Interventions
While children in the first 3 years of life are more vulnerable to toxic stress, they are also more sensitive to the positive impact of early interventions. Evidence-based interventions are even available for children from newborn to 3 years old. These interventions focus on building buffering relationships and have shown positive impacts on children’s neurodevelopment and long-term mental health. Programs shown to provide neurological benefits for young children include Child–Parent Psychotherapy and Attachment Bio-Behavioral Catch-Up, both of which are available in Minnesota. Designed for children who have experienced past trauma, Child–Parent Psychotherapy focuses on strengthening the primary caregiving relationship (Lieberman & Van Horn, 2008). The Attachment Bio-Behavioral Catch-Up intervention program is aimed at first-time mothers as well as children experiencing trauma, impaired caregiving, and early caregiver transitions (Dozier & Bernard, 2017).
One thing that most interventions for children during the first few years of life have in common is an emphasis on the relationship between child and caregiver. Specifically enhancing the ability of the parent to help a child when stressed is a central point of the work. Another shared feature is helping to foster a better understanding of a child’s cues to increase the caregiver’s sensitivity to the child’s needs. Applying these concepts to working with children in the pediatric setting requires additional understanding of infants and young children in a medical setting. For example, the cues of a premature infant may not look like the cues of an infant born full-term. So in order to best support the family’s understanding of their premature infant’s cues, the provider must be attuned to these differences and adjust the psychoeducation accordingly.
Interventions also have to be modified to be delivered in the medical context. Early childhood mental health was born out of home visits with parents and their children (Fraiberg, Adelson, & Shapiro, 1975) and as a result, many interventions were designed to be provided in the home. Unfortunately for some pediatric patients, their home is the hospital. Nevertheless, these children and their families could very much benefit from these interventions. Providers working in this setting need to be able to be flexible in order to deliver the appropriate support that matches the context. This flexibility can mean including other care providers in the intervention, such as nurses, therapists, and medical doctors. It can also mean being able to provide support in the presence of beeping machines, in small rooms, and using toys that are able to be cleaned to the standards required of pediatric environments. In some cases, it also means providing support to families while wearing a protective mask and gown due to infectious disease precautions, something that takes some getting used to.
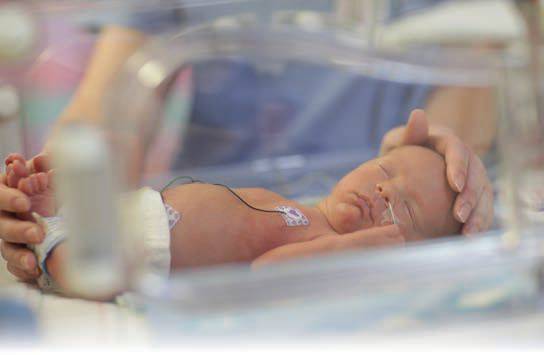
Chronic illness can cause repeated exposure to stressful events such as multiple surgeries, hospitalizations, doctor visits, and blood draws.
Building Buffering Relationships–Sara’s Story
Sara, a 3-month-old baby born with neonatal abstinence syndrome, was admitted to the University of Minnesota Masonic Children’s Hospital Cardiovascular Intensive Care Unit for respiratory distress and risk of infection. She was found to have significant heart defects that caused her main two arteries to be reversed and a hole in her heart that allowed blood to flow in the wrong direction complicated by maternal substance abuse, coarctation of the aorta, and multiple episodes of necrotizing enterocolitis during her post-op course.
Sara fought for her life primarily on her own. Both her parents were young and polysubstance abusers. Her father was never in her life, and her mother suffered from postpartum depression and anxiety disorder. She was going through treatment for a substance use disorder and was not able to care for her daughter. When Sara was born with a positive toxicology screen for opiates, child protection services transferred her to a foster family.
To allow Sara to begin the healing process with her new family, pediatric psychologist Maria Kroupina and her team in the University of Minnesota Birth to Three Clinic and Early Childhood Mental Health Program worked intensely with the child and family to teach the parents how to identify and respond to the baby’s cues of stress. They carefully monitored Sara’s adaptation to her new family with weekly visits in the hospital. During these visits, Dr. Kroupina helped the parents to correctly identify Sara’s distress cues and reinforced their supportive responses to the child as she watched the family engage naturally during the sessions.
At the time of the baby’s discharge, Dr. Kroupina helped the parents with their concerns about the transition to home care. The program team continues to monitor Sara on an outpatient basis to support her social and emotional development by continuing to increase parental sensitivity to cues of stress as well as processing traumatic experiences as a family. This program provides children with health needs and their families’ ongoing support and evidence-based interventions for children during the first 3 years of life. Despite diagnosed serious illness, stressful events related to their medical treatment, and the lack of an adult to mitigate these experiences, the program itself now serves as a buffer against negative impacts. Interventions focused on building buffering relationships therefore reduce the risk of toxic stress and provide new, positive, and healthy directions to explore.
Sara’s early experience clearly placed her at extreme risk for toxic stress and, therefore, poor health and neurodevelopmental outcome. Early intervention was critical to support her health and normal developmental trajectory. We are very excited to provide this caliber of care to our pediatric patients and their families. The program also presents an excellent environment to ask research questions as well as train medical staff. We are poised to do both as our program grows and expands.
Learn More
About the Authors
Maria Kroupina, PhD, is an associate professor in the Department of Pediatrics at the University of Minnesota. The overarching goal of Dr. Kroupina’s combined research-clinical program is to design a research-based clinical program for young children with a history of early adversity and toxic stress. She is the director of a new Birth to Three Clinic and Early Childhood Mental Health Program. This pediatrics program focuses on early identification of high-risk children in order to prevent long-term negative mental health and neurodevelopmental outcomes by providing early intervention. She is a faculty member of the Center for Neurobehavioral Development, University of Minnesota. She was 2009 ZERO TO THREE fellow, and currently she is a member of Academy of ZERO TO THREE Fellows and on the ZERO TO THREE expert training team for the DC:0–5.
Kathryn Elison, MSW, LICSW, is a behavioral health clinician and director of the master’s of social work internship program in the Birth to Three Clinic and Early Childhood Mental Health Program at the University of Minnesota in the Department of Pediatrics. She specializes in working with children from birth to 3 years old with a history of early trauma or adversity, particularly medical trauma. Kathryn has been trained in Child-Parent Psychotherapy, Attachment and Biobehavioral Catch-Up, Trauma Focused Cognitive Behavioral Therapy, and Circle of Security and the FINE Program.
Suggested Citation
Kroupina, M., & Elison, K. (2019). The pediatric Birth to Three Clinic and Early Childhood Mental Health Program: Meeting the needs of complex pediatric patients. ZERO TO THREE Journal, 39(6), 31–35.
References
Boyce, W. T., & Ellis, B. J. (2005). Biological sensitivity to context: I. An evolutionary-developmental theory of the origins and functions of stress reactivity. Developmental Psychopathology, 17(2), 271–301. pmid:16761546
Dozier, M., & Bernard, K. (2017). Attachment and Biobehavioral Catch-up: Addressing the needs of infants and toddlers exposed to inadequate or problematic caregiving. Current Opinion in Psychology, 15, 111–117.
Fraiberg, S., Adelson, E., & Shapiro, V. (1975). Ghosts in the nursery. A psychoanalytic approach to the problems of impaired infant-mother relationships. Journal of the American Academy of Child & Adolescent Psychiatry, 14(3) 387–421.
Gunnar, M. R., & Donzella, B. (2002). Social regulation of the cortisol levels in early human development. Psychoneuroendocrinology, 27(1–2),199–220.
Lieberman, A. F., & Van Horn, P. (2008). Psychotherapy with infants and young children: Repairing the effects of stress and trauma on early attachment. New York, NY: Guilford Press.
Lieberman, A. F., & Van Horn, P. (2008). Psychotherapy with infants and young children: Repairing the effects of stress and trauma on early attachment. New York, NY: Guilford Press.
National Scientific Council on the Developing Child. (2005/2014). Excessive stress disrupts the architecture of the developing brain: Working Paper. Source link.
National Scientific Council on the Developing Child. (2010). Persistent fear and anxiety can affect young children’s learning and development: Working Paper No. 9. Source link.
Osofsky, J. D., & Lieberman, A. F. (2011). A call for integrating a mental health perspective into systems of care for abused and neglected infants and young children. American Psychologist, 66(2), 120–128.
Shonkoff, J. P., & Garner, A. S. (2012). The lifelong effects of early childhood adversity and toxic stress. Pediatrics, 129, 232–246.